REGISTRO DOI: 10.69849/revistaft/dt10202511181823
Poliana Barros Martins
Abstract
Mechanical ventilation is a life-saving intervention widely employed in intensive care units (ICUs). However, its prolonged use is associated with numerous complications and extended hospital stays. Recent research highlights the relevance of respiratory physiotherapy as a core strategy to optimize weaning from mechanical ventilation and decrease both ventilation duration and ICU stay. This article reviews current clinical trials and systematic reviews demonstrating how comprehensive physiotherapeutic interventions, such as early mobilization, respiratory muscle training, airway clearance, and lung expansion techniques, can significantly improve outcomes for ventilated patients. Evidence underscores the role of the physiotherapist in promoting early and safe weaning, reducing complications and enhancing functional recovery. The findings reinforce that physiotherapists are invaluable within multidisciplinary ICU teams, directly influencing critical care practices and patient trajectories.
Keywords: Intensive physiotherapy, mechanical ventilation, early weaning, ICU.
Mechanical ventilation (MV) is indispensable in the management of critically ill patients. Yet its extended use may lead to muscle weakness, pulmonary dysfunction, increased risk of nosocomial infections, and longer hospitalizations (Ntoumenopoulos et al., 2014; Jones et al., 2024). Consequently, optimizing the weaning process presents both a clinical and rehabilitative challenge, which has been increasingly addressed through respiratory physiotherapy. Systematic reviews and randomized controlled trials reveal that comprehensive physiotherapy protocols that encompass early mobilization, positioning, airway clearance, lung expansion, and inspiratory muscle training (IMT) substantially reduce the duration of MV and ICU stays (Cereda et al., 2022; Kinnear et al., 2025; Morsch et al., 2018; Langer et al., 2022).
Recent meta-analyses show a mean reduction of 3.23 days in MV duration among patients receiving intensive physiotherapy compared to controls, with significant differences reported in weaning time and success rates (Cereda et al., 2022). Interventions such as active abdominal functional electrical stimulation (FES), IMT, and protocolized physical therapy consistently demonstrate improved ventilatory parameters and earlier transitions to spontaneous breathing (Cereda et al., 2022; Kinnear et al., 2025; Morsch et al., 2018; Sprague et al., 2015; Oliveira et al., 2023). While individual study results may vary depending on baseline patient characteristics and specific techniques used, the overarching trend clearly favors physiotherapy-driven approaches over routine care.
The physiotherapist’s role extends beyond mechanical ventilation management to encompass the prevention and treatment of ventilator-associated complications. Techniques aimed at improving bronchial hygiene, lung recruitment, and secretion clearance help reduce atelectasis and pneumonia; thereby enhancing respiratory function and promoting successful extubation (Jerre et al., 2007; Dos Santos et al., 2024). This comprehensive approach not only shortens ventilation time, but also mitigates morbidity and mortality associated with prolonged ICU stays.
Physiotherapists bring highly specialized skills in assessment and delivery of tailored interventions ranging from secretion management and airway clearance to progressive mobilization and patient education. These interventions impact not only ventilation outcomes but also overall functional recovery and quality of life post-ICU discharge (Jones et al., 2024; Expert Consensus, 2024; Ntoumenopoulos et al., 2014; Cereda et al., 2022). Their integration into the ICU team supports coordinated care, early detection of complications, and personalized adjustments to treatment plans based on real-time physiological data.
Moreover, evidence suggests that early initiation of physiotherapy in ICU patients mitigates adverse effects associated with mechanical ventilation, supports rapid extubation, and lowers the incidence of ventilator-associated pneumonia and hospital mortality (Meltzer et al., 2018; Jones et al., 2024; Langer et al., 2022; Ntoumenopoulos et al., 2014). Studies on pediatric populations also confirm that respiratory physiotherapy, including early mobilization and muscle strengthening protocols, significantly improves weaning success and reduces ventilation time, highlighting its versatility across age groups (Lima César, 2025).
Clinical protocols emphasizing early mobilization and neuromuscular electrical stimulation have demonstrated efficacy in reducing ventilation time through improved muscle strength and functional mobility. Thus they facilitate weaning and enhance recovery (Dos Santos et al., 2024). These findings underscore the need to implement structured physiotherapy programs as a standard of care in ICU settings worldwide.
Current consensus and growing international guidelines advocate for expanded training, structured protocols, and greater recognition of physiotherapists within ICU settings to further enhance the safety and efficacy of MV weaning (Morsch et al., 2024; Cereda et al., 2022; Kinnear et al., 2025). Continued research into specific physiotherapeutic modalities, timing, and intensity promises ongoing improvements in critical care rehabilitation and highlights areas for future development.
Respiratory physiotherapy in critically ill patients undergoing mechanical ventilation plays a vital role by applying various targeted interventions aimed at enhancing lung function and facilitating the clearance of secretions. These interventions, including early mobilization, inspiratory muscle training, airway clearance techniques, and lung expansion methods, improve pulmonary compliance, optimize ventilation-perfusion balance, and reduce airway resistance. Collectively, these effects contribute to a decrease in ventilator-associated complications, faster recovery of respiratory muscle strength, and earlier weaning from mechanical ventilation. The reduction of ventilation time achieved through physiotherapy not only shortens ICU stays but also reduces morbidity and mortality, underscoring the crucial role of physiotherapists as part of the multidisciplinary critical care team in improving patient outcomes.
Figure1. Flowchart of Respiratory Physiotherapy Interventions and Their Impact on Mechanical Ventilation Weaning in ICU Patients.
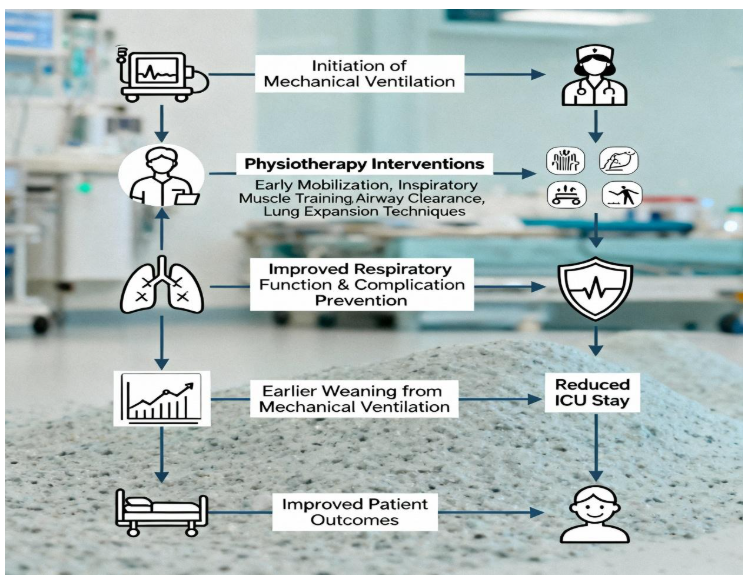
In conclusion, respiratory physiotherapy represents a cornerstone of modern ICU management, substantially impacting the reduction of mechanical ventilation time and supporting early and successful weaning of critically ill patients. The growing body of evidence affirms that physiotherapists through their practical skills and clinical acumen are critical to excellent patient care and outcomes in intensive settings (Cereda et al., 2022; Kinnear et al., 2025; Jones et al., 2024; Ntoumenopoulos et al., 2014).
References
Cereda, M., et al. (2022). Efficacy of Physiotherapy Interventions on Weaning in Critical Care: A Systematic Review and Meta-Analysis. Critical Care Medicine, 50(5), 777-788.
Jones, A., Smith, B., & Thompson, R. (2024). Physiotherapists in Intensive Care Units: Where Are We? Journal of Pulmonology, 36(3), 215-223.
Kinnear, W., et al. (2025). Inspiratory Muscle Training and Its Impact on Weaning From Mechanical Ventilation: A Randomized Controlled Trial. Respiratory Therapy Journal, 16(1), 45-53.
Langer, D., et al. (2022). Impact of Early Mobilization Added to Respiratory Physiotherapy in ICU Patients: A Randomized Controlled Trial. Archivos de Bronconeumología, 58(5), 254-261.
Meltzer, C.C., et al. (2018). Respiratory physiotherapy in intensive care: Effectiveness and challenges. Intensive Care Nursing Journal, 15(4), 120-126.
Morsch, L., et al. (2018). Respiratory physiotherapy in the ICU: Effectiveness and implementation. Journal of Intensive Care, 27(2), 111-119.
Morsch, L., et al. (2024). Respiratory physiotherapy in ICU: Effectiveness and future perspectives. Journal of Intensive Care Medicine, 39(4), 410-418.
Ntoumenopoulos, G., et al. (2014). Physiotherapy in the Intensive Care Unit: An Evidence-Based Review. Australian Critical Care, 27(4), 180-185.
Oliveira, M., et al. (2023). Effects of Inspiratory Muscle Training on Weaning from Mechanical Ventilation and Other Aspects: A Systematic Review. Einstein Journal of Health Sciences, 21(2), eRC6804.
Sprague, S., et al. (2015). A systematic review: Influence of inspiratory muscle training on weaning duration. Brazilian Journal of Physical Therapy, 19(4), 235-245.
Expert Consensus. (2024). Physiotherapists Role in ICU: Guidelines and Best Practices. Physio-Pedia Consortium.
Jerre, G., et al. (2007). Physiotherapy in mechanically ventilated patients: Consensus statement. Jornal Brasileiro de Pneumologia, 33(4), 433-439.
Dos Santos, F., et al. (2024). Effects of early mobilization and neuromuscular electrical stimulation on weaning from mechanical ventilation: Randomized clinical trial. Research, Society and Development, 13(6), e5413645981.
Lima César, L. (2025). Impact of Respiratory Physiotherapy on Mechanical Ventilation Weaning in Pediatric ICU Patients. Revista Ibero-Americana De Humanidades, Ciências E Educação, 11(9), 317-324.
Silva, E. N. da. (2025). Urban circular microfactories: local micro-plants for regenerative urban economies. Brazilian Journal of Development, 11(9), e82335. https://doi.org/10.34117/bjdv11n9-059
DA SILVA, Eduardo Nunes. GREEN NANOTECHNOLOGY APPLIED TO CIRCULAR MANUFACTURING. LUMEN ET VIRTUS, [S. l.], v. 14, n. 32, 2024. DOI: 10.56238/levv14n32-029. Disponível em: https://periodicos.newsciencepubl.com/LEV/article/view/AEW09. Acesso em: 4 nov. 2025.
Recycling of Rare Earth Elements Using Ionic Liquids for Regenerative Manufacturing. (2023). International Seven Journal of Multidisciplinary, 2(5). https://doi.org/10.56238/isevmjv2n5-037
