THE ROLE OF NURSES IN THE STAGES OF THE CHAIN OF SURVIVAL WITH A FOCUS ON PRE-HOSPITAL CARE: A LITERATURE REVIEW
REGISTRO DOI: 10.69849/revistaft/ra10202511111139
Ronaldo Pereira da Silva1, Ruslana Isis Torres Dias1, Denison Pereira da Silva2, Daniele Martins de Lima Oliveira2, Lino Eduardo Farah2; Silvia Roberta Santana Santos Matos1; Patrícia Severino3; Adriana de Jesus Santos3, 1; Marcelo Figueiredo Marques dos Santos 1*, Jennifer Nascimento da Silva3, 2*,
ABSTRACT
Cardiac arrest (CA) is a critical medical emergency with high mortality rates worldwide. In Brazil, the Mobile Emergency Care Service (SAMU) serves as the primary prehospital care (PHC) provider. The effectiveness of CA management depends on the correct implementation of the chain of survival, in which nurses play a vital leadership and coordination role. This study aimed to analyze, through a literature review, the role of nurses in each stage of the chain of survival during prehospital cardiopulmonary resuscitation (CPR). A descriptive and analytical review was conducted using MEDLINE/PubMed, SciELO, LILACS, BDENF, and ScienceDirect databases with the keywords “nursing,” “cardiac arrest,” and “chain of survival” in English, Spanish, and Portuguese. Inclusion criteria considered full-text articles addressing nurses’ roles in prehospital CPR, while experience reports, letters, and editorials were excluded. Six studies met the criteria and were analyzed according to the links of the chain of survival.
Results indicate that nurses are essential in both Basic Life Support (BLS) and Advanced Life Support (ALS). In BLS, they ensure high-quality chest compressions and timely defibrillation. In ALS, nurses coordinate logistics, promote closed-loop communication, prepare and administer medications safely, and accurately document all interventions. Key challenges include maintaining continuous ALS training and improving multidisciplinary team synchronization to optimize patient outcomes. Nurses’ professional practice integrates technical care, management, and humanization, aligning with patient safety and quality goals. Their active participation is crucial to survival and functional recovery in CA cases. Continuing education is fundamental to maintain technical competence and enhance leadership and decision-making abilities. Overall, nurses serve as strategic professionals in prehospital CA care, ensuring the efficiency of the chain of survival and contributing significantly to patient outcomes.
Keywords: Nursing. Cardiac Arrest. Chain of Survival. Pre-Hospital Care.
1 INTRODUCTION
Cardiac arrest (CA) is characterized by the sudden cessation of mechanical cardiac activity, clinically confirmed by the absence of effective circulation (AHA, 2020). It is a highly serious event, responsible for high global mortality, surpassing the sum of several other causes of death, such as cancer and infectious diseases. It is estimated that more than 350,000 cases of CPR occur annually outside the hospital setting in the United States, with a survival rate of only 9.1% until hospital discharge (TSAO et al., 2023). In Brazil, data on incidence remain scarce; however, the highest prevalence of this event occurs in emergency services (DE ALMEIDA et al., 2024).
In Brazil, the Mobile Emergency Care Service (SAMU) is the main reference in prehospital urgent and emergency care (DE OLIVEIRA et al., 2024; DE SA CÂMARA et al., 2024). In this context, in the pre-hospital setting, the application of a chain of survival stands out, defined as a sequence of interdependent interventions aimed at increasing the survival rate in cases of cardiac arrest (DE ARAGÃO et al., 2024; DOS SANTOS et al., 2024; DA SILVA COSTA et al., SILVA, et al., 2025). This chain comprises six links: recognition of CPR, activation of the emergency service, cardiopulmonary resuscitation (CPR), rapid defibrillation, advanced life support, and post-arrest care with comprehensive rehabilitation (DE OLIEVEIRA XAVIER, DE ALMEIDA MARQUES & DE LEMOS, 2025; SILVA et al., 2025).
The effectiveness of the chain of survival depends on the correct and timely execution of each link, with life support provided by trained professionals ensuring qualified interventions until arrival at the hospital, while post-arrest care and comprehensive rehabilitation promote the patient’s functional and neurological recovery (DE FARIAS et al., 2021; PEREIRA et al., 2021; ARAUJO et al., 2022; DE SOUZA et al., 2022; DE LIMA et al., 2024; DE LIMA, DA SILVA PONTES & RAMOS, 2024). Therefore, the work of the multidisciplinary team is essential for the coordination and execution of interventions, with nurses playing a central role in the management and implementation of care actions (GUEDES et al., 2021; DOS SANTOS et al., 2025; MARCELINO et al., 2025).
Nurses have legal, technical, and scientific responsibility in pre-hospital care, as established by Ordinance No. 2,048/2002 of the Ministry of Health (MS). Thus, in order to execute the links in the chain of survival, it is essential that professionals, in addition to knowing each link, understand their specific role and know how to act within their function, applying technical and scientific knowledge, concentration, agility, practical skills, and the ability to make quick and assertive decisions (DA SILVA et al., 2022; DO NASCIMENTO SARAIVA et al., 2021; JUNIOR & DE ARAÚJO, 2023; DA COSTA et al., 2024; FILIPPIN & LISIESKI, 2024).
Studying the role of nurses in this context is important, as these professionals play a role that directly impacts patient survival rates and functional recovery. In addition, this analysis enables the identification of training gaps, the improvement of institutional protocols, and the strengthening of continuing education, contributing to the quality of prehospital care and patient safety (SILVA & LIMA, 2022; VERVLOET et al., 2022; CARDOSO & BARROS, 2024; DA SILVA FERREIRA & FERREIRA, 2024; SCABORA et al., 2024; XAVIER & DE SOUSA, 2024; RODRIGUES et al., 2025).
In view of the above, the present study aims to analyze the role of nurses in the stages of the chain of survival, focusing on pre-hospital care, through a literature review.
2 THEORETICAL FOUNDATIONS
Pre-hospital care (PHC) in Brazil was created to provide immediate care to patients in urgent and emergency situations, even before they arrive at hospitals (MARTINS & PRADO, 2003; RODRIGUES, DA SILVA & GALHARDO, 2024). Inspired by international models, it became a reality with the creation of SAMU in 2003, which structured multidisciplinary teams and standardized protocols, expanding territorial coverage and the effectiveness of care (MALVESTIO & SOUSA, 2024; BARROS et al., 2025).
In this context, nurses stand out as technical leaders, coordinating team actions and ensuring the correct execution of each stage of the chain of survival in cases of cardiopulmonary arrest (DE OLIVEIRA et al., 2022; JÚNIOR & DE ARAÚJO, 2023). Their work integrates science, technique, and humanization, directly contributing to the reduction of mortality, improved survival, and patient safety (REIS & COSTA, 2024).
The history of APH and pre-hospital nursing reflects advances in continuing education, professional integration, and social commitment, consolidating evidence-based practices that save lives and strengthen emergency care (DO CARMO SANTOS et al., 2021; LEAL et al., 2025).
2.1 Pre-Hospital Care Model (APH) in Brazil
PHC refers to the provision of immediate care in urgent and emergency situations outside the hospital environment, focused on acute clinical, traumatic, or psychiatric conditions that, if not treated quickly and appropriately, can result in permanent sequelae or death (MINISTRY OF HEALTH, 2003; TAVEIRA et al., 2021). In this context, APH is an essential component of health services, whether public or private, as it ensures an effective response to critical situations (DE ALMEIDA et al., 2020; DOS SANTOS et al., 2023; COSTA et al., 2024). In Brazil, the Ministry of Health adopted the French model as a reference, implementing the Mobile Emergency Care Service (SAMU) in 2003 (RAMOS & SANNA, 2005; MACHADO, SALVADOR & O’DWYER, 2011; NUNES, DA SILVA & JORGE, 2022).
The service has a hierarchical organization, with a Medical Regulation Center responsible for answering calls, triaging, and dispatching teams (DINIZ et al., 2023; DOS SANTOS-RODRIGUES, MONTEIRO-BATISTA & LAUDARES-KAWAGUCHI et al., 2024). Vehicles are classified according to the complexity of the care required and equipped for advanced interventions, with doctors, nurses, nursing technicians, and driver-paramedics, consolidating an integrated, multiprofessional, and standardized model of pre-hospital care in Brazil (FORASTIERI FILHO et al., 2022; MENDES et al., 2023). SAMU also coordinates with referral hospitals and other health services, ensuring an efficient flow of patients (LIMA et al., 2022; MELO et al., 2023; MARCUSSI, et al., 2024).
The SAMU service is activated by calling 192 (VIEIRA, DE BRITO MEIRA & DOS SANTOS MARINHO, 2021; MALVESTIO; SOUSA, 2022). Calls are initially received by Medical Regulation Assistant Technicians (TARM) and forwarded to the medical staff at the Regulation Center, who determine the most appropriate team and arrange for the patient to be transported to the appropriate hospital (DE OLIVEIRA MARQUES ET AL., 2021; VIEIRA, DELL’AGNOLO, 2022; AZEVEDO, 2023; CARRETTA et al., 2025; DE BARROS PRETTI et al., 2025).
The service uses different types of transport, selected by the coordinating physician according to the severity, urgency, and access conditions (SOUZA et al., 2013). Motorcycle ambulances allow for rapid transport for early treatment, while ambulances are classified as Basic Support Units (BSU), Intermediate Life Support (ILS), and Advanced Support Units (ASU) (CHEVONIK et al., 2021; DO NASCIMENTO SARAIVA et al., 2021; DE AZEVEDO FILHO et al., 2022; TOFANI et al., 2022; DO MONTE et al., 2024). In addition to land vehicles, SAMU employs air ambulances, such as helicopters, and water ambulances, such as the ambulancha (BALDOINO, et al., 2023; NUNES et al., 2023; HERMILLY et al., 2023; ARCURI et al., 2024). This diversity ensures broad territorial coverage, optimizes response time, and promotes better clinical outcomes (DE SA CÂMARA et al., 2024).
The implementation of SAMU with the consolidation of APH in Brazil had an impact on the healthcare system (OLIVEIRA, O’DWYER & NOVAES, 2022). Among the main results, we can mention the reduction in mortality in accidents and clinical emergencies, resulting from rapid and specialized care at the scene of the incident, as well as a decrease in hospital overcrowding (NUNES CONCEIÇÃO et al., 2024; PRANDO et al., 2024). Among the incidents attended by the system, it is observed that medical emergencies represent the highest demand (FRÓES et al., 2022).
Given this scenario, a study conducted by Almeida et al. (2016) and Santos-Rodrigues et al. (2024) reports that among the calls handled by SAMU 192, clinical incidents predominate.
2.1.1 Clinical calls in the PHC
In the context of Brazilian emergency medical services, clinical care accounts for the majority of cases handled by SAMU (CUNHA et al., 2021; FORASTIERE FILHO et al., 2022; JUNIOR & DE ARAÚJO, 2023). These cases include acute medical conditions such as hypertensive crises (HC), acute myocardial infarction (AMI), stroke (CVA), and acute respiratory failure (ARF), which, if not treated quickly and appropriately, can progress to cardiopulmonary arrest (GUEDEs et al., 2022; KURTZ & MARTINS, 2022; LIEBICH et al., 2023; CAVALCANTE et al., 2024; DE BARROS et al., 2025; HONORATO et al., 2025).
Data from the Araguaína City Hall (TO) indicate that 50% of the incidents attended by SAMU in 2023 were clinical in nature, a percentage similar to that observed in the Federal District (60%), highlighting the relevance of the service in responding to acute clinical situations (ARAGUAÍNA CITY HALL, 2024; FEDERAL DISTRICT STATE HEALTH SECRETARIAT, 2024). Thus, certain clinical conditions are more likely to progress to cardiopulmonary arrest (CPA), with AMI being the most frequently reported cause, followed by hemorrhagic stroke, ARF, severe hypertensive crises, and severe infections, as evidenced in studies shown in Table 1 (DA SILVA et al., 2024; DE OLIVEIRA et al., 2025; LUDWIG et al., 2025; SILVA et al., 2025).
Table 1 – Studies that analyzed the main clinical conditions associated with progression to cardiopulmonary arrest (CPA) in prehospital care in Brazil.
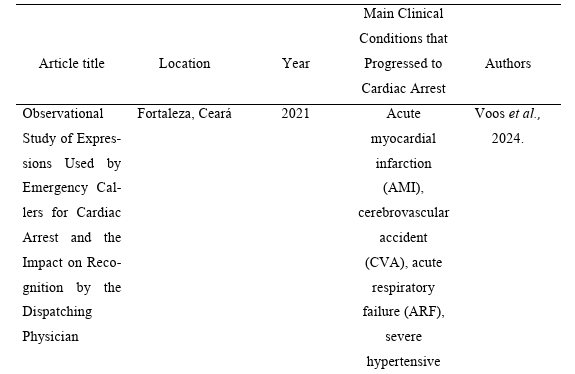


Early intervention in cases of cardiac arrest is recognized as a determining factor for survival and reduction of neurological sequelae (GUIMARÃES et al., 2024; BRANDÃO, MESSAC & SANTOS, 2025; DE OLIVEIRA XAVIER, DE ALMEIDA MARQUES & DE LEMOS, 2025). The literature reports that every minute of delay in starting cardiopulmonary resuscitation reduces the patient’s chances of survival by approximately 7 to 10% (DA SILVA VARÃO et al., 2024; PORTO et al., 2024; ). In this sense, the importance of rapid identification and immediate application of basic life support measures is emphasized, since the agility of the health team’s response, combined with the continuous training of professionals, is a fundamental element in ensuring the effectiveness of the chain of survival (SOUSA, DE CARVALHO BORGES & VELOSO, 2021; JUNIOR & DE ARAÚJO, 2023; SOUZA et al., 2024; Sampaio et al., 2025).
3.2 Chain of Survival in CPR Care
The chain of survival is recognized as a structured model to guide rapid and effective interventions in response to cardiac arrest (SCOBORA et al., 2024). Introduced by the AHA in 1990, the chain of survival has been continuously applied and updated, reflecting scientific advances and adaptations to different clinical contexts (AHA, 2020; PERKINS et al., 2021). Currently, the literature describes two distinct models of the chain of survival: a unified model, focused on the care of adult and pediatric patients in in-hospital and out-of-hospital settings, and another specific to neonatology, considering the physiological and care particularities of this age group—this update was published in October 2025 (AHA, 2025).
Until September 2025, the literature described the chain of survival as consisting of six distinct models: two focused on adult patients (in-hospital and out-of-hospital), two on pediatric patients (in-hospital and out-of-hospital), one for drowning victims, and one specifically for the neonatal population (PAULA et al., 2021; COSTA et al., 2023; PORTO et al., 2023; DE ALVARENGA et al., 2025; DOS SANTOS et al., 2025).
This differentiation is justified by the particularities of pediatric and neonatal care, as both require specific adaptations for the age group (DE MORAIS SILVA et al., 2025) CPR in children often occurs secondary to respiratory failure and shock, while neonatal CPR results from physiological changes specific to the perinatal period, requiring different protocols adapted to the cardiopulmonary fragility and organic immaturity of the newborn. (CAMILO & DE BARROS, 2024; DANTAS et al., 2025; LIMA et al., 2025).
Thus, in drowning victims, the etiology is also primarily associated with respiratory causes, reinforcing the need for immediate rescue ventilation as an initial measure, similar to what is recommended for pediatric care (DE BRITO et al., 2024; DOS SANTOS et al., 2025). In adults, where cardiac causes predominate, the chain of survival prioritizes the immediate initiation of high-quality cardiopulmonary resuscitation and early defibrillation, as these interventions are directly associated with increased survival rates (DE LIMA NETO et al., 2021; GUEDES et al., 2021; ACOSTA-GUTIÉRREZ et al., 2022; DE LIMA, DA SILVA PONTES & RAMOS, 2024).
However, the unification of the chain of survival was defined by the American Heart Association (AHA) with the aim of simplifying and improving CPR care, establishing a more cohesive and easy-to-apply protocol for all first responders, from laypeople to healthcare professionals, with benefits that include improved survival outcomes and ease of training (AHA, 2025).
3.2.1 Stages of the Chain of Survival
The chain of survival consists of six interdependent links, which must be followed in a sequential and orderly manner, ensuring the effectiveness of care at each stage (PAULA et al., 2021; DE CÁSSIA BITENCOURT & RENNÓ, 2023; MITIDIERI, BERTOLIIN & GABRIEL, 2025).
The first link in the chain of survival refers to early recognition of CPR and activation of emergency services, with the recommendation to identify three signs: unconsciousness, absence of a central pulse, and absence of breathing (DOS REIS et al., 2025). In this first link, it is also recommended to call the emergency services, ensuring that the victim receives appropriate professional care as soon as possible (QUILICI et al., 2019; DE ARAGÃO et al., 2024). After identifying CPR, it is essential to start therapy immediately (NACER, SOUZA & MIRANDA, 2023).
Initial treatment corresponds to the second link in the chain of survival, and chest compressions should be started according to a specific protocol in order to ensure quality CPR for the patient (POMPERMAIER, BALENA & GUINZELLI SILVA, 2020). When available, an automated external defibrillator (AED) or cardioverter should be used; in general, an AED can be operated by anyone, while a cardioverter requires guidance from a medical professional, representing the third link in the chain of survival (RODRUIGUES et al., 2022; PEREIRA et al., 2024).
The fourth link in the chain of survival refers to advanced life support (ALS) in CPR, while the first three links correspond to basic life support (BLS), which can be performed by both laypeople and specialized professionals (CARVALHO et al., 2020; DA SILVA et al., 2020; LANDA & FERREIRA, 2020; PELEK, FERREIRA & MÜLLER, 2021; SÁ et al., 2022; DE BESSA et al., 2023). ALS, in turn, should be performed exclusively by trained professionals (Schlinz et al., 2025).
With the presence of a specialized team, the fourth link corresponds to the SAV, enabling the adoption of invasive procedures and the use of specific medications to reverse the condition (BASTO et al., 2020; DE LIMA et al., 2024; PEREIRA et al., 2024; DO NASCIMENTO et al., 2025). During this period, the patient may have two possible outcomes: death or the return of cardiac and respiratory functions (PAULA et al., 2021; BONÉ, LOUREIRO & BONITO, 2022; DE MIRANDA et al., 2023; BRAGA et al., 2024; PRADO et al., 2024). When vital functions return, the fifth link in the chain of survival can be applied, corresponding to postarrest care, with the aim of stabilizing the patient, preventing complications, and reducing the risk of further cardiopulmonary arrest (Da Silva et al., 2021; Avila; Lucindo & Barbosa, 2024; Benítez-Verón; Ordano-Palacios & Ortega-filártiga, 2024. De Lima et al, 2025).
The sixth link was incorporated into the AHA CPR guidelines in 2020, but it is still little known by professionals or, in some cases, neglected (DA SILVA DUARTE et al., 2021; De ALVARENGA et al., 2025). This link, called recovery, involves the physical, neurological, and emotional rehabilitation of the patient after cardiopulmonary arrest, focusing on improving quality of life, preventing new events, and social reintegration (BENETTI et al., 2021; MENDES et al., 2021; DA SILVA OLIVEIRA et al., 2024; DE OLIVEIRA XAVIER, DE ALMEIDA MARQUES & DE LEMOS, 2025).
This entire process is only possible through the integrated and coordinated efforts of a multidisciplinary team, whose collaboration is essential to ensure safe, humane, and evidencebased care (SILVA et al., 2020; CUNHA et al., 2021; DE ARAÚJO PORTO et al., 2023). In this context, APH, the effectiveness of all links in the chain of survival depends on the joint action of doctors, nurses, nursing technicians, and trained emergency medical technicians (ROSA et al., 2020; SOUSA, TELES & OLIVEIRA, 2020; DO NASCIMENTO SARAIVA et al., 2021; DE LIMA TORRES et al., 2023). When properly trained, these professionals ensure the execution of all stages of the chain of survival (GONCALVES, 2023; DOS SANTOS CARVALHO et al., 2024).
3.3 Role of the Multidisciplinary Team in PCR Care
In the context of CPR care, the multidisciplinary team is made up of different professionals who work in an integrated and coordinated manner, generally consisting of nurses, nursing technicians, and physicians (SILVA et al., 2020; CAMILO & DE BARROS, 2024). However, in some regions of the country, physical therapists are also part of the multidisciplinary team providing care for sudden cardiac arrest in the prehospital setting (DE SOUSA, 2021).
Each member of the multidisciplinary team performs complementary and interdependent functions, which are fundamental to the effective implementation of SBV and/or SAV (VASCONCELLOS et al., 2021; DE CAMARGO ROSA, SANTOS & ZIMMER, 2023).
The effectiveness of this joint action is directly related to the second International Patient Safety Goal, which advocates safe and effective communication among healthcare professionals, highlighting the importance of closed-loop communication during CPR (ALCÂNTARA et al., 2025; LOPES et al., 2025; PORTELA et al., 2025). Thus, in addition to clear communication, the team must have leadership capable of promoting quick and accurate decision-making, the proper distribution of tasks, and maintaining synchrony among its members—determining factors for the success of resuscitation and patient survival (WINTER et al., 2023; BRETANHA et al., 2024; TURRA et al., 2024).
However, challenges and limitations, such as lack of ongoing training, scarcity of resources, and difficulties in team synchronization, can compromise the effectiveness of care, reinforcing the need for training strategies and standardized protocols to optimize multidisciplinary performance in the context of CPR (PASSARINI et al., 2021; CANÁRIO et al., 2024; DIAS et al., 2024).
Within the team, the physician leads resuscitation, performing rapid assessment of the patient, making complex clinical decisions, prescribing medication, and performing advanced interventions such as orotracheal intubation and defibrillation using a cardioverter, when indicated (BERNOCHE et al., 2019; GUIMARÃES et al., 2020; VINAGRE, 2024). When integrated into the prehospital CPR care team, the physical therapist performs functions aimed at maintaining the patient’s ventilation and oxygenation (DA SILVA et al., 2025).
Nursing professionals are responsible for the initial assessment of the patient, monitoring vital signs, performing effective chest compressions, ventilation with a bag-valvemask (BVM) device, and preparing medications for administration when necessary (DE PAULO et al., 2021; DE OLIVEIRA SANTOS et al., 2023; HALEY, 2023; SANTOS et al., 2023). In addition, nurses coordinate the logistics of care, ensuring the organization of materials, the proper positioning of the patient, and the synchronization of the team (TACAHASHI, PIRES & SILVANIO, 2025).
Dentro da equipe de enfermagem, o enfermeiro atua como líder e referência técnica, supervisionando os procedimentos realizados pelos técnicos e garantindo que as práticas estejam alinhadas aos protocolos de reanimação, promovendo a segurança do paciente e a efetividade do atendimento à PCR (De Jesus; Pfaffenbach; Gomes, 2024; Dos Santos et al., 2025).
3.4 Role of the nurse in CPR care
Ensuring compliance with resuscitation protocols in the context of APH is essential to guarantee patient safety and the effectiveness of interventions during CPR (ALBINO, 2024; REIS & COSTA, 2024; JÚNIO et al., 2025). In this scenario, nurses play an essential role in the rigorous implementation of these protocols, ensuring that each stage of Basic and Advanced Life Support is performed in accordance with current technical and scientific guidelines, promoting standardization, quality of care, and better clinical outcomes (SANTANA et al., 2021; DA SILVA CASTRO et al., 2025; DE SOUZA MARQUES et al., 2025).
Thus, nurses can play an active and continuous role in monitoring actions from the initial recognition of cardiopulmonary arrest to the coordination of interventions performed (LOPES & NOGUEIRA, 2021; VERVLOET et al., 2022; DA SILVA GOULART, LIMA & DIAS, 2025). As the technical leader of the multidisciplinary team, nurses play a strategic role in distributing and organizing tasks, monitoring the execution of maneuvers, and ensuring that chest compressions, ventilation, and defibrillation occur in a synchronized and efficient manner, ensuring the quality of care and increasing the chances of successful resuscitation (STEFANI, 2021; SILVA & LIMA, 2022; DE OLIVEIRA SANTOS et al., 2023; COUTINHO DA COSTA et al., 2024; MARQUES & RODRIGUES, 2025).
Nurses, as higher-level professionals, promote closed-loop communication, ensuring the integration of team actions during CPR (DE SOUZA LIMA et al., 2024). In accordance with institutional protocols, they can administer previously established medications, in addition to performing private procedures that contribute to the effectiveness of care. They are also responsible for nursing progress and the accurate recording of interventions, ensuring traceability, patient safety, and continuity of care (SILVA & DONDA, 2022; DE FRANÇA & DA SILVA TENÓRIO, 2023; MINUZZI & DA SILVA PEREIRA., 2023; DE FARIAS et al., 2024; PEREIRA et al., 2024; DO NASCIMENTO et al., 2025).
The effective performance of nurses in the context of CPR in a pre-hospital setting depends directly on continuous training and periodic CPR training (DE AZEVEDO & DE MEDEIROS, 2021; DE OLIVEIRA, 2025; DE SOUSA FERREIRA et al., 2025). In the mobile emergency service, nurses also play a role alongside the multidisciplinary team, linked to the Permanent Health Education Center (NEPS), which enables the constant updating of knowledge, familiarization with protocols, and improvement of leadership and decision-making skills (DO CARMO SANTOS et al., 2021; DUTRA et al., 2024). This ongoing training strengthens nurses’ technical competence and clinical reasoning, directly reflecting on the quality of care and increased survival rates in pre-hospital emergencies (DE AZEVEDO & DE MEDEIROS, 2021; DA SILVA PRADO & DA SILVA, 2023).
It should be noted that the work of nurses in CPR care, in addition to providing assistance, also has social and institutional relevance (MÜNCHEN, QUINTANA & VASCONCELLOS, 2022; JÚNIOR & DE ARAÚJO, 2023). This practice is directly associated with the Sustainable Development Goals (SDGs), specifically SDG 3 – Good Health and Wellbeing, as it contributes to reducing mortality from preventable causes through qualified and timely interventions (MENEGAZ, TRINDADE & SANTOS, 2021; MARTINS et al., 2024; MORAES FILHO & TAVARES, 2024). In addition, it aligns with SDG 4 – Quality Education, by promoting continuing education and ongoing professional development for healthcare teams, and SDG 8 – Decent Work and Economic Growth, by valuing qualification, safety, and technical improvement in the workplace (DOS CARMO MENEGAZ; DE LIMA TRINDADE & DOS SANTOS, 2021; MARTINS et al., 2022; COSTA et al., 2023; TAMINATO, FERNANDES & BARBOSA, 2023).
Therefore, understanding and describing in detail each intervention performed by nurses during cardiopulmonary resuscitation is essential to recognize the scope of their work, optimize clinical outcomes, and strengthen evidence-based practices in prehospital emergency care (CARVALHO, 2021; DOS SANTOS CARVALHO et al., 2024; DE OLIVEIRA XAVIER, DE ALMEIDA MARQUES & DE LEMOS, 2025; DE SOUSA FERREIRA et al., 2025; LEAL et al., 2025).
3 METHODOLOGY
This study is characterized as a descriptive and analytical literature review, whose objective was to analyze the role of nurses in the stages of the chain of survival, focusing on prehospital care.
The following terms were used as descriptors, combined with Boolean operators AND/OR: “nursing,” “cardiac arrest,” and “chain of survival” in Portuguese, English, and Spanish. The research was conducted through a bibliographic survey of the following electronic databases: Medical Literature Analysis and Retrieval System (MEDLINE/PubMed), Scientific Electronic Library Online (SciELO), Latin American and Caribbean Health Sciences Literature (LILACS), Nursing Database (BDENF), and ScienceDirect, selected for their broad representation of relevant scientific journals in the areas of nursing, urgent care, and emergency care.
The inclusion criteria used to select the studies were scientific articles published between any period with full texts available; studies that addressed the role of nurses in prehospital care in situations of cardiopulmonary arrest. Exclusion criteria were studies reporting experiences, letters to the editor, editorials, and duplicate works in the databases consulted.
The selection analysis consisted of a critical reading of the titles and abstracts, followed by a full reading of the eligible articles to verify their relevance to the proposed theme. Initially, 1.762 articles were found; after applying the inclusion and exclusion criteria, six studies comprised the final sample of this review.
The selected articles were analyzed and their information categorized according to the links in the chain of survival, allowing the identification of the main care and management activities of nurses, as well as the challenges faced and the strategies used to optimize survival and the quality of prehospital care.
For data organization and analysis, Microsoft Excel® was used for tabulation and categorization of information, and Origin® (2018) was used for graphing. The illustrations and flowcharts were created to represent the methodology in Figure 1.
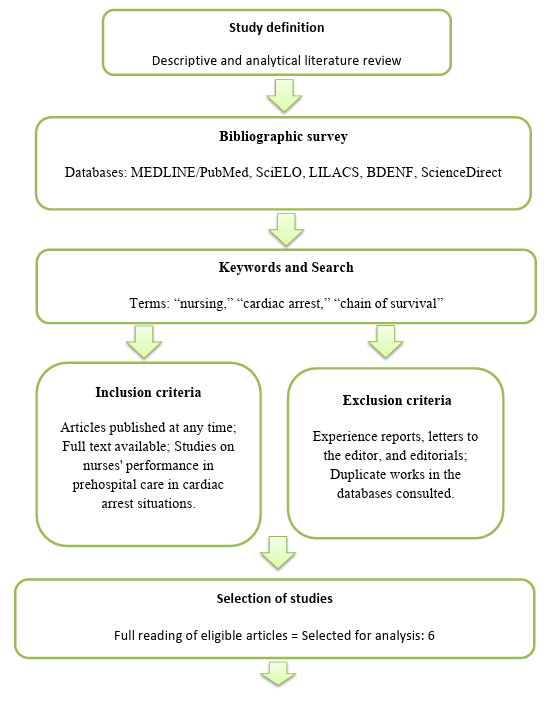

Figure 1: Flowchart of the study methodology.
4 RESULTS AND DISCUSSIONS
The descriptors previously defined in the methodology were applied in combination, using Boolean operators, in the three languages, and could be used in trios, pairs, or individually. This approach allowed us to select a wide variety of studies related to the theme.
The articles that met the inclusion criteria were organized in Table 2, considering the title, objective, year of publication, main results, and authors.
Table 2: Characteristics of the studies included in the review, with information on title, objective, year of publication, main results, and authors.
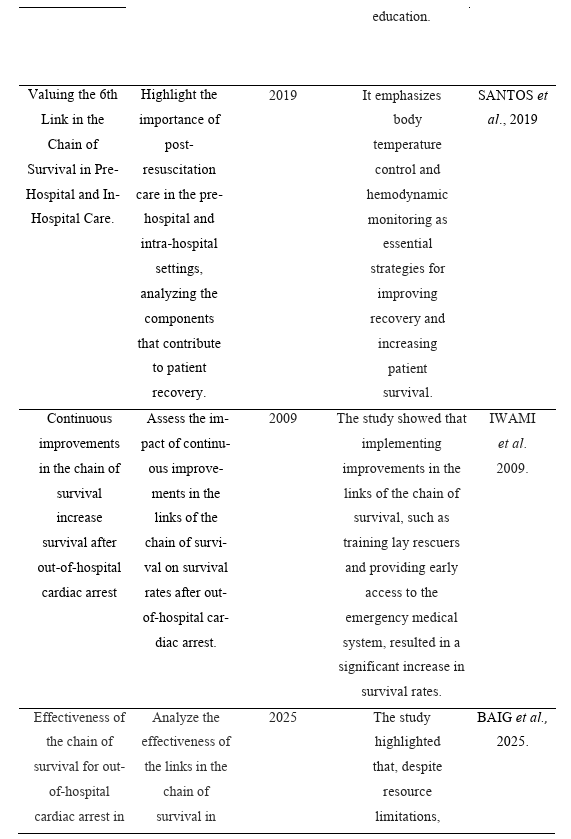
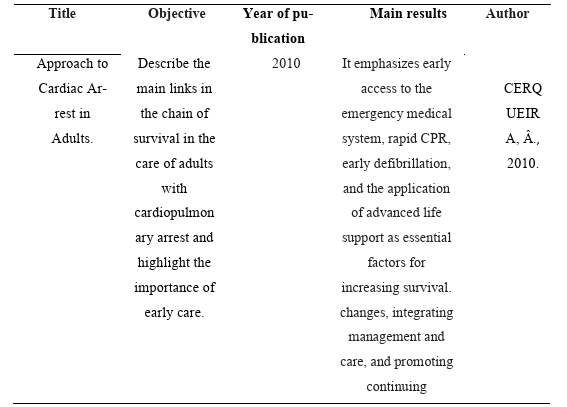

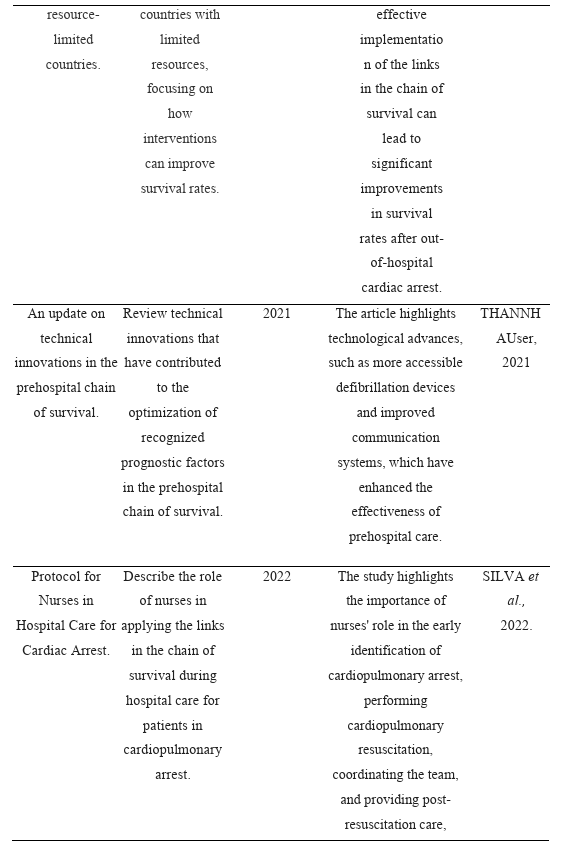

The analysis of the studies included in the review highlights the central role of nurses in the stages of the chain of survival, especially in the context of prehospital care. The study by Cerqueira (2010) emphasizes that early access to the emergency system, rapid CPR, early defibrillation, and the application of advanced life support are factors that affect increased survival in adults with cardiopulmonary arrest. These findings reinforce the importance of trained nurses and continuing education for rapid identification and intervention in emergencies.
Santos et al. (2019) highlight post-CPR care, emphasizing that body temperature control and hemodynamic monitoring are essential strategies for optimizing patient recovery. These data reinforce the concept that the role of nurses is not limited to initial resuscitation, but extends to continuous management and critical assessment of the patient’s clinical condition.
Studies by Iwami et al. (2009) and Baig et al. (2025) demonstrate that improvements in the chain of survival, even in resource-limited settings, have an impact on survival rates. Training lay rescuers, rapid access to emergency services, and proper application of the steps in the chain of survival are critical to the effectiveness of prehospital care. These findings indicate that nurses play a strategic role in both coordinating resources and implementing standardized clinical protocols.
Thannhauser (2021) emphasizes that technological innovations, such as accessible defibrillation devices and improved communication systems, enhance the effectiveness of prehospital care, suggesting that nurses should be up to date with new technologies and integrate them into clinical practice. Silva et al. (2022) demonstrate that nurses play a leading role in the early identification of cardiopulmonary arrest, the performance of CPR, team coordination, and post-resuscitation care, highlighting the relevance of each link in the chain of survival.
The analysis of Table 2 showed that, although the studies address the chain of survival in the prehospital context and mention the functions performed by nurses, none presented a detailed and exclusive analysis of the role of nurses in each specific link in this chain.
Thus, this study is unique in proposing a systematic analysis of the role of nurses in each stage of the chain of survival, filling important gaps in the existing literature and providing guidance for nurses to provide more efficient and safer care.
The first link in the chain of survival, according to the updated international recommendations of the American Heart Association (2025), corresponds to early recognition of cardiac arrest and immediate activation of the emergency system In this context, the literature describes that nurses play a role in quickly identifying clinical signs of circulatory and respiratory collapse, establishing efficient communication with the dispatch center, and guiding initial procedures for the lay population (SILVA & LIMA, 2022; SCOBORA et al., 2024).
A study conducted by Bernoche et al. (2019) highlights the importance of this response time, demonstrating that for every minute a patient remains in cardiac arrest without effective assistance, there is an approximate 10% reduction in the chance of returning to spontaneous circulation. This finding reinforces the importance of immediate and technically qualified action by nurses, who, by recognizing CPR early and providing appropriate support, contribute significantly to increasing survival rates and reducing associated neurological damage.
In the study by Guedes et al. (2021), the importance of recognizing cardiac arrest is widely highlighted as a determinant for the patient’s prognosis. The authors emphasize that early identification of the event, followed by requesting help from the healthcare team and immediately initiating cardiopulmonary resuscitation maneuvers, are essential for a better prognosis. The article also stresses that continuous training of the nursing team, through periodic training and professional updating, improves the quality of care provided in cardiac arrest, which includes the ability to recognize the event quickly.
Furthermore, in the integrative review conducted, a knowledge gap was observed among professionals regarding the recognition and management of cardiac arrest—implying that recognition is not always immediate or adequate. Therefore, the authors conclude that the reinforcement and repetition of training at intervals no longer than six months favor the team’s preparation to act promptly, reducing the time for identification and initiation of resuscitation maneuvers, reinforcing the need for continuous training to ensure an efficient response and reduction of mortality from cardiac arrest.
The results obtained in this study indicate that the presence of qualified nurses with upto-date training in basic and advanced life support is directly associated with a reduction in response time and an increase in survival rates (DA SILVA & DA SILVA, 2023; DEGRAF & BERTOLIN, 2023). These findings reinforce the evidence demonstrating that the clinical competence and rapid judgment of the nurse in the pre-hospital setting are crucial for the timely activation of available resources, optimizing the care flow and strengthening the effectiveness of the chain of survival (SILVA et al., 2025).
The updates from the AHA (2025) and European emergency networks highlight the expanded role of the nurse in the first link of the chain of survival, driven by the incorporation of digital technologies and intelligent regulation systems. The incorporation of tools such as real-time geolocation, rapid response applications, and tele-guidance platforms has allowed nurses to act as a mediating link between the citizen and the regulation center, performing telemonitoring, providing guidance via video or audio, and applying standardized digital protocols for the early recognition of cardiorespiratory arrest and the initiation of resuscitation maneuvers before the arrival of the mobile team (SOUSA & SILVA, 2018; LIMA & MATOS, 2022).
In the context of the first link in the chain of survival, the nurse occupies a strategic position both in the dispatch center, guiding the population during the recognition of cardiac arrest, and in the training of communities capable of acting early. During telephone assistance, the nurse uses clinical triage protocols and qualified listening to interpret the findings reported by laypeople—such as absence of breathing, cyanotic coloration, and lack of response—safely guiding the caller in identifying cardiac arrest (SILVA et al., 2024; REIS & PEREIRA, 2025).
In parallel, this professional acts as a permanent educator, promoting actions aimed at the population to teach about the recognition and basic cardiopulmonary resuscitation. In addition, they teach about recognizing warning signs, such as chest pain and syncope. Recent studies demonstrate that regions with greater involvement of nurses in educational activities and in healthcare regulation show a significant reduction in response time and a higher survival rate until the first shock, reinforcing the impact of this integrated approach between assistance and education (OLIVEIRA et al., 2024; NAKAMURA, 2025).
The second link in the chain of survival refers to the performance of CPR maneuvers, essential for maintaining cerebral and circulatory perfusion until the arrival of advanced support (AHA, 2025). The effective performance of this link depends directly on the adequate fulfillment of the first link, that is, the rapid recognition of cardiorespiratory arrest and the immediate activation of the emergency system (AHA, 2020; LIMA, PONTES & RAMOS, 2024; CHIARELLI et al., 2025).
In this context, the nurse must perform or ensure that the rescuer responsible for chest compressions maintains the appropriate quality of the maneuvers, ensuring that the technical gesture reproduces the physiological role of the heart—acting as systole during compression and as diastole when the chest returns completely to its original position (NASCIMENTO et al., 2021; OLIVEIRA, MOREIRA& MARTINS, 2022; DA SILVA et al., 2025). This alternation is essential to promote effective circulation, optimize coronary and cerebral blood flow, and increase the chances of return of spontaneous circulation (NORTE, 2022).
According to De Lima, da Silva Pontes & Ramos (2024), high-quality CPR is a determining factor in increasing survival rates in cases of cardiopulmonary arrest, especially among adults and the elderly. The authors state that the early and correct performance of chest compressions, with adequate depth, frequency, and chest recoil, is directly associated with maintaining coronary and cerebral perfusion. The study reinforces that continuous training of healthcare professionals is essential to ensure that the maneuvers are performed according to updated guidelines, reducing technical errors and optimizing clinical outcomes. Thus, highquality CPR is configured not only as a technical competence but as a fundamental practice for the effectiveness of care in critical situations.
Recent studies have shown that the survival rate is directly associated with the quality of CPR (DA SILVA et al., 2025). The study by Vestergaard et al. (2021) showed that adequate chest compression rates and maintaining a chest compression fraction (CCF) above 80% are related to higher 30-day survival rates. The CCF corresponds to the proportion of time the chest is effectively compressed during resuscitation, and is calculated using Formula 1:

In a multicenter simulation study, Caregiver Characteristics Associated With Quality of Cardiac Compressions demonstrated that factors such as muscle fatigue and anthropometry of healthcare professionals negatively impact the depth and rate of compressions, with the Borg Scale being a useful parameter to measure the subjective perception of effort during the procedure.
Additionally, simulation and training research, such as the study Simulation-Based Training in High-Quality Cardiopulmonary Resuscitation Among Intensive Care Unit Providers, demonstrated a significant improvement in depth, rate, and compression fraction parameters after educational interventions with real-time feedback, reinforcing the importance of evidence-based pedagogical strategies. These findings are corroborated by the scoping review “The Optimal Strategy for Training Cardiopulmonary Resuscitation for Healthcare Professionals”, which indicates that periodic training, realistic simulations, and the use of feedback devices are crucial to ensure high-quality CPR.
The following graph was created from the average values described in the analyzed studies, comparing the main parameters of CPR before and after training. The results presented include compression rate (compressions per minute), average depth (in millimeters), chest compression fraction (CCF, in percentage), and perceived exertion (Borg Scale). The visualization allows observation of the direct impact of the training on improving technique and reducing the physical effort perceived by the professionals, reinforcing the effectiveness of educational strategies in improving CPR, Figure 2.
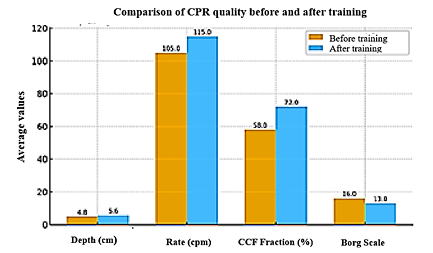
Figure 2 – Comparison of CPR quality parameters before and after simulated training with real-time feedback. A significant improvement is observed in the compression rate (compressions per minute), average depth (mm), and chest compression fraction (CCF, %), as well as a reduction in perceived exertion according to the Borg Scale. The data were obtained from the average of the results reported by Vestergaard et al. (2021), Caregiver
Characteristics Associated With Quality of Cardiac Compressions (2020), Simulation-Based Training in HighQuality Cardiopulmonary Resuscitation (2022) and The Optimal Strategy for Training Cardiopulmonary Resuscitation for Healthcare Professionals (2023).
In addition to high-quality chest compressions, in this link of the chain of survival, the nurse must ensure adequate ventilation during cardiopulmonary resuscitation, using the bagvalve-mask (BVM) device with correct technique and efficient sealing (BAESSO, AMORIM & JÚNIOR, 2025). The professional needs to assess and maintain the recommended ratio of 30 compressions to 2 ventilations (when there is no definitive airway), and must also ensure visible chest rise with each insufflation, without causing hyperinflation or gastric distension (DE LIMA TORRES et al., 2023; NICOLADELi, 2023).
For a high-quality CPR scenario to be effective, it is fundamental that the nurse has a previously trained rapid response team, acting under their coordination (CARDOSO, BAROOS & PARAGUEM, 2024; MENIGUIN et al. 2024). It is the nurse’s responsibility to manage all events occurring during resuscitation, making real-time corrections whenever necessary (DOS SANTOS et al., 2025). Regarding ventilation, the nurse must supervise or directly perform the management of the device, ensuring that the equipment is complete, with a mask and selfinflating bag of a size compatible with the patient and properly connected to the gas panel, guaranteeing an oxygen flow of 15 liters per minute (DA CONCEIÇÃO LUCENA et al., 2022; BROWN III et al., 2024; DE ASSIS et al., 2025; PEREIRA et al., 2025).
In the context of ventilation with a non-definitive airway, the nurse must ensure the correct execution of airway opening techniques before each ventilation (DA SILVA et al., 2024; DE LIMA, DA SILVA PORTE & RAMOS, 2024). In trauma patients, the jaw thrust maneuver is recommended, while in cases of clinical etiology, proper positioning should be achieved through the chin lift and head extension maneuvers (PHTLS, 2023). The October 2025 protocol brought a relevant update by exceptionally allowing the performance of the chin lift in trauma patients when no other maneuver proves effective in restoring airway patency (AHA, 2025).
At this point in the chain, the nurse’s differential is the capacity for critical thinking to assess the need for insertion of the Guedel oropharyngeal airway, ensuring the maintenance of a patent airway (DA SILVA et al., 2024; DO SANTOS CLAUDIANO, LOPES & FIORIN, 2024; DA SILVA GOULART, LIMA & DIAS, 2025). The nurse, in their proactivity, ensures that the suction equipment is pre-prepared and available to allow for an immediate response to possible obstructions by secretions (DO NASCIMENTO et al., 2023; TACAHASHI, PIRES & SILVANIO, 2025).
The third link in the chain of survival corresponds to early defibrillation, a fundamental step in the management of cardiac arrest that aims to restore sinus cardiac rhythm through the application of a controlled electric shock to the victim’s chest and the rescuer’s compression action (CORREA et al., 2025; DEGANI et al., 2025; DOS SANTOS et al., 2025). Defibrillation is considered the most effective intervention when performed early, as it helps the rescuer reverse arrhythmias and restore spontaneous circulation (ROSC) with a lower chance of neurological deficit (MITIDIERI, BERTOLIN & GABRIEL, 2025; PEREIRA et al., 2025; ZOSCHKE et al., 2025).
In this context, the nurse acts both in the direct operation of the equipment (Automated External Defibrillator – AED, or cardioverter) and in coordinating the resuscitation team, ensuring that the equipment is available, functional, and used quickly and safely (SILVA et al., 2021; DA SILVA OLIVEIRA et al., 2024; RODRIGUES & BARROS, 2024).
The AED is equipment that can be used by the entire nursing team and also by laypeople, provided they are trained, as stipulated in Brazilian legislation (BRAZIL, 2018). Regarding the use of defibrillators, COFEN Resolution No. 704/2022 standardizes the actions of the professional nurse during cardiac arrest, ensuring legal support for the use of these devices (WINTER et al., 2023). Article 1 of the resolution allows the nursing team to use the AED, while Article 2 establishes that, in the absence of this equipment, the management of the manual defibrillator (cardioverter) to administer the electric shock is exclusive to the nurse (COFEN, 2022; CORREA et al., 2025). The standard further reinforces that the nurse is responsible for coordinating defibrillation actions, guaranteeing the quality and safety of care, provided that they are duly trained and supported by institutional protocols that guide the practice (COFEN, 2022).
Studies have highlighted the relevance of training nursing professionals in the recognition and early execution of defibrillation, especially in cardiac arrest situations (BORGES et al., 2025). Research conducted in countries such as Finland, Hong Kong, and Saudi Arabia has shown a significant increase in the confidence and technical skills of nurses after educational interventions focused on CPR and the use of a defibrillator (FINN, 1996; KO et al., 2011; ALANAZI et al., 2021). Figure 3 below summarizes these findings, showing the percentage increase in nurses confident in performing early defibrillation before and after training, reinforcing the importance of continuous training strategies for improving clinical outcomes.
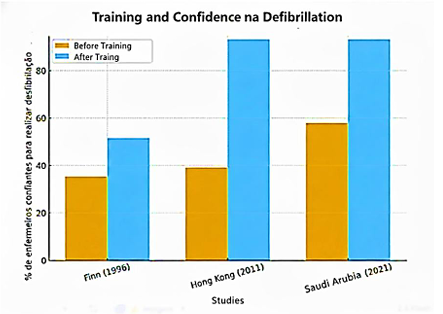
Figure 3: Impact of training on early defibrillation. The graph demonstrates the percentage increase in nurses who reported feeling confident in performing early defibrillation after participating in specific CPR training. A significant increase in self-confidence and readiness of professionals is observed after the training, indicating that theoretical and practical training directly contributes to the safety and effectiveness of the response in situations of cardiorespiratory arrest. Source: Adapted from Finn (1996), Ko et al. (2011) and Alanazi et al. (2021).
Electrocardiogram (ECG) interpretation is a fundamental skill for nurses in urgent and emergency situations, especially during cardiac arrest (DA SILVA BEZERRA, SECATI & MELO, 2021; DE ARAÚJO PINTO et al., 2024; FELIPE et al., 2025). Understanding cardiac tracings makes it possible to identify shockable and non-shockable rhythms, guiding management and the correct use of the defibrillator (DE SOUSA FERREIRA et al., 2025; SAMPAIO & PENHA, 2025). The nurse must recognize, at a minimum, the sinus rhythm and distinguish the main cardiac arrest rhythms, such as asystole, pulseless electrical activity (PEA), ventricular fibrillation (VF), and pulseless ventricular tachycardia (VT), ensuring rapid and effective interventions (LIMA, 2021; BRITO et al., 2022; DE OLIVEIRA SANTOS et al., 2023; DE OLIVEIRA XAVIER, DE ALMEIDA MARQUES & DE LEMOS, 2025). This competence ensures safe decisions and reinforces the nurse’s leading role in coordinating actions during emergencies (LOPES & NOGUEIRA, 2021; SILVA & LIMA, 2022).
The efficient performance of the nurse in this role requires critical thinking, technical mastery, and leadership, allowing defibrillation to occur within the ideal time (between 3 and 5 minutes after collapse) as recommended by the protocols (ACADROLI & NOBRE, 2023; WALENDOWSKY, 2025). After the shock, the professional must ensure the immediate resumption of chest compressions and meticulously record all events, times, and clinical responses (MASTINE, 2023; GOGOLA et al., 2023; DOS SANTOS et al., 2024).
Therefore, early defibrillation represents the turning point in the chain of survival, situated between Basic Life Support (BLS) and Advanced Life Support (ALS) (MENDES et al., 2021; CARDOSO & BARRO, 2024; DOS SANTOS et al., 2024; AHA, 2025). Up to the third link, the actions are included in the context of BLS, and when performed correctly and coordinated by a properly trained nurse, they improve the results of cardiopulmonary resuscitation, directly contributing to increased survival rates and a reduction in post-cardiac arrest complications (DE SOUSA et al., 2024; DO NASCIMENTO et al., 2024; CHIARELLI et al., 2025).
Advanced Life Support (ALS) encompasses a set of interventions performed by healthcare professionals with specific training and technical qualifications, aimed at restoring spontaneous circulation and stabilizing the patient after cardiorespiratory arrest (Pereira et al., 2024). At this stage, advanced airway management techniques are employed, in addition to the administration of medications, constituting the fourth link in the chain of survival (DE MATTOS OLIVEIRA et al., 2024; SANTOS et al., 2024).
Regarding the nurse’s role in this link of the chain of survival, when ventilation with a BVM (bag-valve-mask) does not adequately ventilate the patient, the nurse can use a laryngeal mask, a supraglottic device indicated to ensure a definitive airway in emergency situations, especially during CPR (SILVA et al., 2022; KUNZ et al., 2022; DE OLIVEIRA et al., 2025). The legal basis for the use of the laryngeal mask by nurses is found in COFEN Resolution No. 641/2020, which establishes the competence of nursing professionals to use extraglottic devices, including the laryngeal mask, in situations of imminent risk of death.
When the nurse performs ventilation using a supraglottic device, such as the laryngeal mask, they must coordinate the entire team, ensuring that chest compressions are continuous, interrupting only when changing the rescuer responsible for the compressions (PEREIRA et al., 2025). In addition to performing or supervising ventilation, performed synchronously every six to eight seconds, the nurse must correctly position the team members, ensuring visibility, adequate access to the patient, and efficient execution of the maneuvers (GUIMARÃES, 2023; DOS REIS VIEIRA et al., 2024).
In a study conducted by Kunz et al. (2022) on nurses’ perceptions regarding the use of the laryngeal mask, the majority of participating nurses demonstrated satisfactory knowledge of the clinical indications for its use, with 80% reporting correct identification of situations in which the device should be employed. However, this same study indicates that only 30% of professionals had received prior training on its use, and the same percentage stated that they possessed knowledge about the legislation regulating the use of the device by nurses. These data reveal a discrepancy between theoretical knowledge and practical training, reinforcing the importance of implementing continuous training programs focused on airway management and safe and effective action during clinical emergencies.
Finally, if the attending physician decides that endotracheal intubation is necessary to secure the airway at this time, the nurse must prepare all the necessary materials and test them beforehand, including endotracheal tubes, connectors, and auxiliary devices (LIMA et al., 2021). In addition, they must assist the physician during intubation, perform pre-oxygenation of the patient, and provide guidance on the appropriate apnea time during the procedure (FRISANCO et al., 2022; BOMFIM et al., 2025; MARQUES, 2025).
Concurrently with airway support measures, the nurse’s role in the administration and management of medications during cardiac arrest is essential for the success of resuscitation (SCABORA et al., 2024; CAVALHEIRI, FARIAS & BATISTELLA, 2025). The professional must prepare, check, and administer the prescribed medications according to institutional protocols, rigorously monitoring their effects and ensuring patient safety, using closed-loop communication to ensure clarity and efficiency throughout the entire procedure (DE CAMARGO BENDINELLI & HANGAI, 2024; DO NASCIMENTO et al., 2025; GASPAR & LIMA, 2025; PORTELA et al., 2025).
Prior to the administration of medications during CPR, it is the responsibility of the nurse or nursing team to establish safe and functional venous access, ensuring the availability of necessary medications during resuscitation (ALBINO, 2024; NASCIMENTO & LIMA, 2025). If peripheral venous access is not feasible, it is the nurse’s responsibility to perform intraosseous access, a procedure supported by COFEN Resolution No. 704/2022, which regulates the performance of nursing professionals in advanced life support interventions, including the appropriate route for drug administration in critical situations (COFEN, 2022).
The nurse’s responsibility during this phase of CPR also includes performing the correct aseptic technique in the aspiration and preparation of medications, ensuring the accuracy of doses and maintaining the sterility of the procedure (BARRETO et al., 2025; BROCCA et al., 2025). It is the nurse’s responsibility to verify the compatibility of the drugs, perform dilution according to medical recommendations, manufacturer’s instructions, or institutional protocols, and ensure the proper identification of syringes, preventing medication errors in a context of high complexity and urgency (DA SILVA et al., 2025; DE SOUSA FERREIRA et al., 2025). Thus, the nurse’s actions must be based on good clinical practices, scientific support, and adherence to the regulations of the Federal Council of Nursing (COFEN, 2022), ensuring quality and safety in all phases of resuscitation.
The nurse, as a member of the resuscitation team, must possess in-depth knowledge of pharmacokinetics and pharmacodynamics, as stipulated in COFEN Resolution No. 564/2017, which establishes the competencies of the nursing professional in the process of prescribing, preparing, and administering medications (COFEN, 2017). This theoretical and practical mastery allows for an understanding of the mechanism of action, indications, contraindications, and adverse effects of the drugs used during cardiopulmonary resuscitation (CPR), ensuring safe, effective, and evidence-based interventions (CASTILHO & FONSECA, 2025; DE SOUZA, DE LIRA SILVA & DE OLIVEIRA NÓBREGA, 2025; GALÁN MORALES, 2025; PEREIRA et al., 2025; RONCONI, 2025).
Among the most commonly used drugs, the nurse must have complete mastery over the main drugs used in cardiopulmonary resuscitation, such as epinephrine, amiodarone, and lidocaine (DOS SANTOS PEREIRA, DA SILVA LOPES & DOS SANTOS PEREIRA, 2021; CAVALHEIRI, FARIAS & BATISTELLA, 2025). Epinephrine is considered the first-choice agent, acting as an alpha and beta adrenergic agonist, promoting peripheral vasoconstriction and increased coronary and cerebral blood flow (DA COSTA JUNIOR et al., 2022; AGOSTINHO et al., 2024). Its administration should occur at a dose of 1 mg every 3 to 5 minutes, intravenously (IV) or intraosseously (IO), according to AHA guidelines (2025). It is fundamental that the nurse knows how to correctly manage the dose and administration interval to ensure therapeutic efficacy and patient safety (Morais et al., 2025; Pereira et al., 2025).
The endotracheal route, previously used for drug administration during CPR, has been gradually abandoned due to low pharmacokinetic predictability and variable absorption, resulting in lower plasma concentrations compared to the intravenous (IV) and intraosseous (IO) routes (WELL & TANG, 2000). The ERC guidelines, updated by Soar et al. (2021), recommend the preferential use of the IV/IO routes for drug administration during CPR. In the Brazilian context, Resolution COFEN No. 704/2022 supports duly trained nurses performing intraosseous access in emergency situations. This recommendation reflects the pursuit of greater therapeutic effectiveness and better clinical outcomes, as demonstrated in the data presented in Table 3.
Table 3: Comparison between drug administration routes during CPR and their clinical outcomes.

In the pre-hospital setting, even in the physical absence of a physician, the current protocol authorizes the use of epinephrine by the nurse, since there is remote medical supervision through radio communication, guaranteeing technical and legal support for the intervention (COUTINHO, 2011; DE ALMEIDA & ÁLVARES, 2019). After administering the drug, the nurse should be aware that it is recommended to infuse a 20 mL bolus (flush) of saline solution to optimize drug dispersion (PIACEZZI et al., 2021). In cases of peripheral venous access, the limb with the access should be elevated for at least 10 seconds to favor venous return and ensure adequate circulation of the medication (ÁVILA, LUCINDO & BARBOSA, 2024; DOS SANTOS CLAUDIANO, LOPES & FIORIN, 2024).
Furthermore, in situations of verbal prescription via radio, the nurse may administer antiarrhythmic drugs, provided they correctly identify the rhythm on the ECG and know the doses, indications, and appropriate times of administration (DOS SANTOS et al., 2024; SILVA et al., 2025). In these cases, amiodarone, a class III antiarrhythmic and first-choice drug, is indicated after the third rhythm check when a sustained shockable rhythm is identified, being administered at a dose of 300 mg in a bolus, with the possibility of repeating 150 mg (CARBAJO MARTÍN & PÉREZ MIRANDA; ARACIL, 2022; MIRANDA & GIRON, 2022).
Lidocaine, a class IB antiarrhythmic, can be used as an alternative, at a dose of 1 to 1.5 mg/kg, with a repetition of half the initial dose if necessary (LÓPEZ-HERCE et al., 2022; CAMPOS et al., 2024; CAVALHEIRI, FARIAS & BATISTELLA, 2025).
Therefore, pre-hospital nurses must continuously update their knowledge and skills in advanced life support, mastering invasive procedures and pharmacological interventions, ensuring safe and efficient care aligned with current guidelines, thus strengthening the role of the nurse as an essential professional in the chain of survival (FORMOSO MACHADO et al., 2021; PEREIRA et al., 2024; DA SILVA et al., 2025; DE LIMA et al., 2025; GONÇALVES, 2025; SANTANA et al., 2025).
After advanced life support interventions, the patient may progress to two main outcomes: return of spontaneous circulation (ROSC) or death (Laporte et al., 2021; Dos Santos & Costa, 2022). ROSC indicates the success of resuscitation maneuvers and is directly associated with the quality of actions at each link in the chain of survival, from early recognition to appropriate pharmacological management (DOS SANTOS et al., 2024; MATEUS et al., 2024; PEREIRA et al., 2025). Even after the return of circulation, the patient remains in a critical condition and requires immediate post-cardiac arrest care, focused on hemodynamic stabilization, maintenance of oxygenation, and neurological protection, constituting the fifth link in the chain of survival (SOUSA, DE CARVALHO & VELOSO, 2021; DA SILVA & DOS SANTOS MAIA, 2022).
According to the updated 2025 guidelines of the European Resuscitation Council (ERC) and the AHA, post-cardiac arrest care should be performed systematically and multidisciplinarily (AHA, 2025; ERC, 2025). The nurse is responsible for continuously monitoring hemodynamic parameters, ensuring the maintenance of mean arterial pressure (MAP) ≥ 65 mmHg and oxygen saturation between 92-98%, adjusting vasoactive infusions and ventilatory support as prescribed by the physician (ARANTE; FERREIRA, 2022; De VASCONCELOS TEIXEIRA et al., 2024; DE OLIVEIRA XAVIER, DE ALMEIDA MARQUES & DE LEMOS, 2025; GOMES et al., 2025).
In ventilation and oxygenation, the nurse is responsible for ensuring adequate oxygen titration, preventing hypoxia and hyperoxia, as well as evaluating signs of respiratory distress and blood gas changes – when available in the pre-hospital setting (PEREIRA, 2024; SCABORA et al., 2024). In temperature control, the nurse rigorously monitors body temperature and applies measures to prevent fever, according to protocols (AHA, 2025; BRAGA et al., 2025). They also actively participate in the identification and communication of possible causes of cardiac arrest, collaborating with the medical team in conducting complementary examinations and emergency interventions when available in the pre-hospital setting (MIRANDA & GIRON, 2022; KINAMA et al., 2023; PEREIRA et al., 2025).
During the neuroprognostication process, the nurse in the pre-hospital setting plays a crucial role in immediate neurological monitoring, observing the level of consciousness, motor response, and presence of seizures, intervening when necessary (BRAGA et al., 2025; GOMES et al., 2025). Furthermore, they are responsible for glycemic control, medication administration, detailed recording of interventions, and providing support to the family (AMORIN, 2025; SILVA et al., 2025). Thus, the nurse assumes an essential role in the fifth link of the chain of survival, ensuring the continuity of qualified care and contributing directly to the recovery and prognosis of the post-cardiac arrest patient in the pre-hospital setting (DA SILVA et al., 2021; DE LIMA et al., 2025).
The final stage of post-cardiac arrest care in the pre-hospital environment involves the safe and rapid transfer of the patient to the hospital setting, ensuring the continuity of intensive care and the maintenance of clinical stability (DE LIMA et al., 2024; DA SILVA et al., 2025). In this context, the nurse is responsible for ensuring continuous monitoring during transport, maintaining ventilatory support, infusions, and a patent venous access, as well as communicating the clinical condition and interventions performed to the receiving hospital team in a structured manner (DE MELO et al., 2023; PEREIRA & PAES, 2023).
The effective transfer of information and continuous patient monitoring reduce the risks of instability and data loss, strengthening the integration between pre-hospital and in-hospital care (MELO et al., 2023; MENOLLI, SANTANA & MARTINS, 2025). In this way, the nurse’s role in post-cardiac arrest care ensures a safe and efficient transition for the critically ill patient (RIBEIRo et al., 2023; CHIARELLI et al., 2025), consolidating the sixth link in the chain of survival, focused on rehabilitation and continuous monitoring of the patient after hospital discharge.
Although the sixth link in the chain of survival, described in international guidelines, includes recovery and rehabilitation – post-hospital discharge follow-up – it does not directly address the pre-hospital context (REIS et al., 2024; PEREIRA et al., 2025; PORTO et al., 2025). However, its understanding is fundamental for nurses to recognize the importance of continuity of care, ensuring that the actions performed in the initial care contribute to the client’s prognosis and recovery (MEDEIROS et al., 2024; DA SILVA et al., 2025; MELO et al., 2025). According to the AHA (2025), the sixth link involves continued neurological and physical support, multidisciplinary follow-up, control of reversible causes, in addition to physical, cognitive, and psychological rehabilitation, culminating in the individual’s reintegration into daily and social life.
However, it should be noted that pre-hospital care can also contribute to the effectiveness of the sixth link in the chain of survival (VINCENTE et al., 2024). The nurse’s role in the Mobile Emergency Medical Service can be crucial in ensuring continuity of care through detailed recording of interventions performed and structured communication with the hospital team (ARAÚJO, OSPINA & ARAÚJO, 2025).
A study conducted by Joshi and co-authors (2022) analyzed 721 cardiac arrest survivors with the objective of evaluating rehabilitation interventions aimed at the neurological, physical, and psychological function of the patients. A meta-analysis indicated a moderately high effect for improvement in neurological function, while the effects on quality of life were inconclusive. The results reinforce the importance of multidisciplinary rehabilitation, including nursing, in post-cardiac arrest follow-up. Furthermore, we identified gaps in the literature that justify further studies on specific nursing care in this phase.
Furthermore, the guidance and support provided to the family during care reinforce the human and educational character of the care, aligning with the principles of the sixth link (AHA, 2025; SILVA et al., 2025). A study conducted by Barbosa (2022) highlighted that humanization in pre-hospital care involves not only the correct execution of techniques but also attention to the emotional aspect of the patient and family members, promoting welcoming, empathy, and clear communication. The study emphasizes that humanized practices can reduce suffering and improve the care experience, even in critical situations such as cardiac arrest, reinforcing the need to integrate technical and human care in nursing training.
Thus, even without directly executing the rehabilitation process, the pre-hospital nurse plays an important role as a transitional link between immediate survival and the patient’s overall recovery, strengthening the integration between care levels and the continuous line of care (BELGA, SILVA & JORGE, 2023; TORRENTE et al., 2024; DA SILVA et al., 2025).
Pre-hospital care in cardiac arrest situations presents challenges that directly impact the quality and continuity of care, such as the scarcity of material resources, workload, failures in communication between care levels, technical and scientific deficits of the professional, and limited time for critical decisions (DA SILVA OLIVEIRA et al., 2025; JÚNIOR et al., 2025; SANTIAGO Júnior et al., 2025). These conditions can compromise the proper execution of protocols and hinder the comprehensiveness of care (NASCIMENTO & LIMA, 2025). Faced with these challenges, it becomes essential to invest in strategies that strengthen the role of the nurse and improve the performance of emergency teams, highlighting continuous training and technical-scientific training (GUEDES et al., 2021; GIL et al., 2025).
The theoretical and practical mastery of basic and advanced life support, combined with periodic training in realistic simulations and the updating of international protocols, enhances response capacity and reduces errors during care (MOUTINHO BOSSO et al., 2022; MROCZINSKI et al., 2023). Furthermore, continuous improvement strengthens clinical reasoning and evidence-based decision-making in highly complex situations, promoting more favorable prognoses and consolidating the image of the nurse as an essential professional in the care of critically ill patients (DOS SANTOS MOTA et al., 2022; CAMBOIM et al., 2023).
In this context, when the nurse clearly recognizes their role in each link of the chain of survival, from the first to the sixth link, they optimize response time and reduce the occurrence of errors in the care process (DEGRAF & BERTOLIN, 2023; CARDOSO & BARROS, 2024; CHIARELLI et al., 2025). This integrated approach, based on updated protocols, contributes to more assertive interventions, favoring hemodynamic stability, the return of spontaneous circulation, and the reduction of neurological sequelae (DA SILVA et al., 2023; ZOSCHKE et al., 2025). Thus, technical-scientific knowledge combined with rapid and safe decision-making reinforces the nurse’s leading role as an essential element in the chain of survival, directly impacting more positive prognoses and the quality of life of patients experiencing cardiac arrest (COSTA et al., 2025; DA SILVA et al., 2025).
5 CONCLUSION/FINAL CONSIDERATIONS
The combined application of descriptors in three languages, using Boolean operators, enabled the selection of studies addressing the chain of survival in the pre-hospital context. It was evident that, although several studies describe the chain of survival in general, none presented a detailed and exclusive analysis of the nurse’s role in each specific link, making this study unique in proposing a systematic evaluation of this participation, filling gaps in the literature and offering support for a more efficient and safe nursing practice. Based on the analysis performed, it is evident that the nurse’s role in the stages of the chain of survival in pre-hospital care is crucial for the quality of care and for reducing mortality from cardiorespiratory arrest. The evidence indicates that, by following international recommendations, the nurse can play a central role from the early recognition of the event and activation of the emergency system to the execution of basic and advanced life support interventions, also contributing to the continuity and effectiveness of care. However, it is observed that the practice faces challenges, such as limited material resources, workload, and deficiencies in communication between care levels, factors that compromise the agility and coordination of actions. In this context, the importance of continuing education, systematic training in basic and advanced life support, and strengthening the clinical and managerial competencies of the nurse are emphasized, indispensable elements for patient safety and the optimization of results. Thus, the nurse’s role must go beyond the technical aspect, integrating the dimensions of assistance, management, and humanization, in order to ensure comprehensive care that also includes welcoming and guiding the family, reinforcing the ethical and humanized character of professional practice in the pre-hospital context.
Considering the gaps identified in the literature, future studies are planned that will explore a qualitative approach seeking to contribute to understanding the perceptions, difficulties, and strategies of nurses working in out-of-hospital cardiopulmonary arrest situations, providing support for the improvement of protocols and continuous training policies. Furthermore, experimental studies and applied field research aiming to validate specific protocols for nurses’ actions at each link in the chain of survival will be conducted, ensuring standardization and safety in clinical practice. Additionally, research will investigate aspects related to humanization, communication with family members, and stress management among professionals to strengthen the understanding and performance of nursing in the pre-hospital setting.
REFERECES
A DE ALMEIDA, T. A. P., FARIAS, M. D. D. S. B., REIS, A. J. A., DAMASCENA, D. E. L., DE ARRUDA RODRIGUES, J. M., COSTA, M. B. G., & BARBOSA, M. F. L. Theoretical knowledge of the nursing team in the care of cardiorespiratory arrest in adults. Research, Society and Development, v. 13, n. 4, p. e7913445573-e7913445573, 2024.
A SILVA CASTRO, M. D. F., BARCELOS, F. V. L., DE SOUZA VEIGA, I. H. P., BARBOSA, P. D. S. M., MENEZES, T., & COSTA, V. B. Factors involved in the impracticality of patient safety protocols by healthcare professionals. Electronic Journal Health Collection, v. 25, n. 6, p. e20437-e20437, 2025.
ACADROLI, R. A., & NOBRE, L. F. M. The level of knowledge of students regarding basic life support in cases of cardiorespiratory arrest at a university in Western Paraná. Brazilian Journal of Implantology and Health Sciences, v. 5, n. 3, p. 451-471, 2023.
ACOSTA-GUTIÉRREZ, E. G., ALBA-AMAYA, A. M., RONCANCIO-RODRÍGUEZ, S., & NAVARRO-VARGAS, J. R. Postpartum cardiac syndrome in hospitalized adult patients. Colombian Journal of Anesthesiology, v. 50, n. e972, p. 1-14, 2022.
ALBINO, G. R. A. Tactical pre-hospital care: pre-hospital care in military operations. IberoAmerican Journal of Humanities, Sciences and Education, v. 10, n. 4, p. 1320-1334, 2024.
ALCÂNTARA, R. B., PIUZANA, E. D. O. F., STERNICK, E. B., IBIAPINA, C. D. C., SCALABRINI NETO, A., & ALMEIDA, A. M. Validation of a specific checklist for the management of cardiorespiratory arrest: shockable rhythms. Brazilian Journal of Medical Education, v. 49, n. 3, 2025.
ALMEIDA, P. M. V. D., DELL’ACQUA, M. C. Q., CYRINO, C. M. S., JULIANI, C. M. C. M., PALHARES, V. D. C., & PAVELQUEIRES, S. Analysis of SAMU 192 services: Mobile component of the emergency care network. Anna Nery School, v. 20, n. 2, p. 289-295, 2016.
ALSABRI, MAH, ALQEEQ, BF, ELSHANBARY, AA, SOLIMAN, Y., ZAAZOUEE, MS, & YU, R. Impact of training on nurses’ confidence and performance in early defibrillation: a Saudi Arabian study. Saudi Journal of Nursing and Health Care, v. 4, n. 2, p. 78–85, 2021.
AMERICAN HEART ASSOCIATION. Destaques das Diretrizes da American Heart Association 2025 para RCP e ACE. [S. l.]: American Heart Association, 2025.
AMERICAN HEART ASSOCIATION. Highlights of the 2025 American Heart Association Guidelines Update for CPR and ECC. Dallas: AHA, 2025.
AMORIM, E. D. Neurological prognosis after cardiorespiratory arrest. 2025.
ARANTES, J. E. G., & FERREIRA, T. V. Nursing care in the management of cardiorespiratory arrest. Health Vales Journal, v. 1, n. 1, 2022.
ARAUJO, N. R. D., ARAÚJO, R. A. D., MORETTI, M. A., & CHAGAS, A. C. P. Training and retraining on cardiopulmonary resuscitation for nursing: a theoretical-practical intervention. Journal of the University of São Paulo School of Nursing, v. 56, p. e20210521, 2022.
ARAÚJO, T. P. R.; OSPINA, Y. P.; ARAÚJO, M. R. The challenges of medical regulation in pre-hospital emergency services. Current health landscape, p. 45,2025.
ARCURI, R., DE SOUZA FERREIRA, D., BELLAS, H. C., DE ANDRADE, B. B. L., MASSON, L. P., VIDAL, M. C. R., CARVALHO, P. V. R., & JATOBÁ, A. Ergonomics and resilience engineering in the formulation of guidelines for the SAMU 192 vessel service. Ergonomic action magazine, v. 14, n. 2, p. 0-0, 2024.
ÁVILA, D. C., LUCINDO, M. C. R. N., & BARBOSA, K. J. Simulation as a teachinglearning strategy for nursing professionals in emergency units. Contemporary Journal, v. 4, n. 10, p. e6356-e6356, 2024.
AZEVEDO, C. R. F. D. A. Medical Regulatory Assistant Telephone Operator. In: Medical Regulatory Assistant Telephone Operator. p. 48-48, 2023.
BAESSO, I. B., AMORIM, A. A., & JÚNIOR, C. B. Non-invasive ventilation in the preoxygenation of critically ill patients: a literature review. Pedagogical Notebook, v. 22, n. 1, p. e13083-e13083, 2025.
BAIG, M. N. Effectiveness of chain of survival for out-of-hospital cardiac arrest in resourcelimited countries. The Lancet Regional Health – Americas, 10, 100011, 2025.
BALDOINO, M., HERKRATH, F., HORTA, B., & GARNELO, L. Lifestyles and work organization of community health agents in river units in the Amazon. Work, Education, and Health, v. 21, p. e02470231, 2023.
BARBOSA, C. S. The humanization of nursing care in pre-hospital care during cardiorespiratory arrest: a narrative review. Pontifical Catholic University of Goiás, 2022.
BARBOSA, N. A. C., & BRESSANIN, H. O. Challenges in the transition of care between healthcare networks. Brazilian Congress of Enterostomal Therapy, 2025.
BARRETO, A. L., DINIZ, A. M., RAMOS, S., & MARTINS, L. Prevention of infection in the preparation and administration of intravenous medications. Millenium-Journal of Education, Technologies, and Health, n. 18e, p. e39130-e39130, 2025.
BARROS, S. S. C., DA SILVA COSTA, F., BARROSO, T. N. S., DOS ANJOS, F. D. S. M., COELHO, S., DA SILVA, F. L., & MACEDO, E. F. S. The importance of a multidisciplinary team in the care of polytraumatized patients in emergency and urgent care services.. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 1, p. 755-762, 2025.
BASTOS, T. D. R., SILVA, M. S. A. D., AZEVEDO, C. P., BORDALLO, L. E. D. S., & SOEIRO, A. C. V. Medical students’ knowledge of basic life support in the management of cardiorespiratory arrest. Brazilian Journal of Medical Education, v. 44, p. e111, 2020.
BELGA, S. M. M. F., SILVA, K. L. D., & JORGE, A. D. Intra-hospital devices and care practices: implications for the comprehensiveness and continuity of care. Text & ContextNursing, v. 32, p. e20230005, 2023.
BENETTI, H. A., CUSTÓDIO, D. C. G. G., DA SILVA, P. R., DE ASSIS SOUZA, L., DA CRUZ, G. S., DO NASCIMENTO, L. S., & CASTILHO, N. G. R. Challenges faced by nurses when dealing with cardiorespiratory arrest in an emergency and urgent care hospital. Brazilian Journal of Development, v. 7, n. 12, p. 112925-112943, 2021.
BENÍTEZ-VERÓN, S. E., ORDANO-PALACIOS, J. V., & ORTEGA-FILÁRTIGA, E. A. Knowledge on cardiopulmonary resuscitation of nursing staff. Scientific journal health sciences, v. 6, p. 1-7, 2024.
BERNOCHE, C., TIMERMAN, S., POLASTRI, T. F., GIANNETTI, N. S., SIQUEIRA, A. W. D. S., PISCOPO, A., & SAKO, Y. K. Update on the cardiopulmonary resuscitation and emergency cardiovascular care guideline of the Brazilian Society of Cardiology2019. Brazilian Archives of Cardiology, 2019.
BERNOCHE, C., TIMERMAN, S., POLASTRI, T. F., GIANNETTI, N. S., SIQUEIRA, A. W. D. S., PISCOPO, A.,& SAKO, Y. K.Update of the Brazilian Society of Cardiology’s Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care – 2019. Brazilian Archives of Cardiology, v. 113, n. 3, p. 449-663, set. 2019.
BOAS, S. M. V., BARRETO, R. S., MATOS, E. P., SOUZA, S. S. S. S. S., FERREIRA, S. M. I. L., MONTEIRO, N. M. A. T., & SANCHES, R. D. C. N. Patient safety strategies in the transition of care: Integrative review. Nursing Brazil, v. 24, n. 4, p. 2736-2778, 2025.
BONÉ, M., LOUREIRO, M. J., & BONITO, J. Basic life support in the 9th grade: Teaching methodologies for student reading comprehension. Boné, 2022.
BONFIM, Í. D., ARAGÃO, I. I., FROZ, A. V. N., BEZERRA, T. M., DE LIMA DIAS, G. G., DA SILVA MARTINS, T., & LOBO, L. F. Specific contexts regarding orotracheal intubation in obese patients. Brazilian Journals in Scientific Research, v. 4, n. 1, p. 24312442, 2025.
BRAGA, R. D. S., SILVA, G. S., KURTZ, P., & TIMERMAN, S. Temperature Management After Cardiac Arrest: A Narrative Review from the Perspective of a Developing Country. Brazilian Archives of Cardiology, v. 122, p. e20240696, 2025.
BRAGA, S. T., DE SENA, A. S. R., NASCIMENTO, L. M. F., BEZERRA, G. D., DE LIMA, V. G., MARCELINO, B. F., SILVA, J. M. F. L., & PINHEIRO, W. R. Analysis of the survival of patients subjected to CPR maneuvers based on the Utstein protocol. Current Nursing Journal in Dermatology. v. 98, n. 2, 2024.
BRANDÃO, A. C. M., MESSAC, D. A., & SANTOS, I. N. Epidemiology of pediatric cardiopulmonary resuscitation. Journal Archives of Health, v. 6, n. 4, p. e3329-e3329, 2025.
BRAZIL. Law No. 13,722, of October 4, 2018. This law makes it mandatory for teachers and staff of public and private basic education institutions and children’s recreation facilities to receive training in basic first aid. Official Gazette of the Union, Brasília, DF, 05 out. 2018.
BRAZIL. Ministry of Health. Mobile Emergency Care Service (SAMU). [cited on: October 26, 2003.
BRAZIL. Ministry of Health. Ordinance No. 2,048 of November 5, 2002. Approves the technical regulations of the National Emergency and Urgency System. Official Gazette of the Union, Brasília, DF, Section 1, p. 66, November 6, 2002.
BRETANHA, A. S. F., FEIJO, C. K., TEIXEIRA, P. H. M., DE ARAÚJO CALAND, F., DOS SANTOS, K. A. V., OLIVEIRA, B., PAIXÃO, G. B., ALVES, J. P. M., COSTA NETO, F. A., CARNEIRO, G. C., SALES, F. C. D., & DIAS, D. M. The importance of training the multidisciplinary team in the face of cardiorespiratory arrest: An integrative literature review. Research, Society and Development, v. 13, n. 10, p. e14131047032e14131047032, 2024.
BRITO, J. S., DE SOUSA, A. A., DE ALMEIDA, S. M. F., DE ALMEIDA, S. M. F., DA SILVA, E. L., DA SILVA, A. M. G., & PASTORE, R. T. Nursing care provided by the nurse during cardiorespiratory arrest in the emergency room. Research, Society and Development, v. 11, n. 15, p. e330111535211-e330111535211, 2022.
BROCCA, E. N., DA ROSA, F. S., DA SILVA FONTANA, T., DA SILVA PIEROTTO, A. A., SCHNEIDER, V., SCHETTERT, M. R., & BARILLI, S. L. S. Patient safety from the patient’s perspective. Electronic Journal Health Collection, v. 25, p. e18805-e18805, 2025.
BROWN III, C. A., SAKLES, J. C., & MICK, N. W.V Walls’ Manual for Airway Management in Emergency Situations. Artmed Publishing House,2024.
CAMBOIM, B. B. P., FERREIRA, I. P., DE OLIVEIRA, V. L. G., DA SILVA, E. L. M. E., DA SILVA, C. C. L. S., DA COSTA CUNHA, K., & DA SILVA, P. O. Teaching advanced life support to nursing students and professionals. Electronic Journal Health Collection, v. 23, n. 12, p. e14702-e14702, 2023.
CAMILO, M. B. A., & DE BARROS, F. F. Competencies for multiprofessional care in pediatric cardiopulmonary resuscitation: perceptions of the nursing team. Space for Health, v. 25, 2024.
CAMPOS, A. P. P., DE SOUZA, B. A., COSTA, D. F., ELIAS, E. B. P., DA SILVA, L. L., CARMONA, M. Y. D. M., & RODRIGUES, W. R. C. Perspectives and challenges of antiarrhythmic drugs: mitigating the risk of proarrhythmia. Epitaya E-books, v. 1, n. 78, p. 13-40, 2024.
CANÁRIO, M. N. M., DA SILVA, A. A., SILVA, A. C., DOS SANTOS BARBOZA, N. M., & DE SOUZA, B. F. N. Technological resources available for improving the cardiopulmonary resuscitation process: an integrative review. JRG Journal of Academic Studies, v. 7, n. 15, p. e151321-e151321, 2024.
CARBAJO MARTÍN, L., PÉREZ MIRANDA, A., & ARACIL, M. C. Advanced cardiopulmonary resuscitation. AMF: Update on Family Medicine, v. 18, n. 4, 2022.
CARDOSO, L., & BARROS, J. Cardiopulmonary arrest: a case study of a rapid and integrated response. In: Contemporary nursing: new challenges, care integration, and care pathway. Digital Scientific Publisher, p. 131-145, 2024.
CARDOSO, L., & BARROS, J. Cardiorespiratory arrest: a case study on a rapid and integrated response. Contemporary nursing: new challenges, integration of care and care pathway, p. 131-145, 2024.
CARRETTA, L. T. A., TEIXEIRA, P. R., COLARES, M. S., DE MARTIM, V. M., MACHADO, W. C., PIMASSONI, L. H. S., NETO, C. D., & DUARTE, S. K. A. Epidemiological Profile and Mapping of Chest Pain in Elderly Patients Treated by SAMU in a Brazilian Capital. Brazilian Journal of Health Review, v. 8, n. 3, p. e79485-e79485, 2025.
CARVALHO, L. R. D., FERREIRA, R. B. S., RIOS, M. A., FONSECA, E. D. O. S., & GUIMARÃES, C. F. Factors associated with lay people’s knowledge of basic life support. Nursing Today of Costa Rica, n. 38, p. 163-178, 2020.
CARVALHO, M. P. S. Impact of the intervention on nurses’ knowledge of adult cardiopulmonary resuscitation. 2021.
CASTILHO, R. P., & FONSECA, J. P. S. The impact of continuing education on medication administration: improvements in nursing practice. Nursing Brazil, v. 24, n. 3, p. 2375-2387, 2025.
CAVALCANTE, F. V., THEODÓRIO, N. E. M., MENDES, M. R. P., & BRANT, J. L. B. SAMU-DF’s perspective on primary care-sensitive conditions in Brazil’s capital. BIUS – Unimotrisaúde Newsletter on Sociogerontology v. 49, n. 43, p. 1-21, 2024.
CAVALHEIRI, J. C.; FARIAS, G. V.; BATISTELLA, A. R. Knowledge of nursing professionals regarding pediatric cardiopulmonary arrest. Paraná Public Health Journal, v. 8, n. 2, p. e1027-e1027, 2025.
CHEVONIK, I. E., MARCONDES, L., DA SILVA, J. C., CORDEIRO, T. L. R., & ALBUQUERQUE, G. M. Profile of services provided by advanced support units of the regional metropolitan SAMU of Paraná. Electronic Health Magazine, v. 13, n. 7, p. e8136e8136, 2021.
CHIARELLI, B. G. N. Cardiopulmonary Resuscitation (CPR): New Protocols and Advanced Techniques. Brazilian Journal of Implantology and Health Sciences, [s. l.], v. 7, n. 2, p. 246-257, 2025.
CHIARELLI, B. G. N., MOTA, A. L. G., GONTIJO, A. F. M., & REZENDE, D. N. Cardiopulmonary Resuscitation (CPR): New Protocols and Advanced Techniques. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 2, p. 246-257, 2025.
COFEN. Resolução nº 704, de 19 de julho de 2022. Normatiza a atuação dos profissionais de Enfermagem na utilização do equipamento de desfibrilação no cuidado ao indivíduo em parada cardiorrespiratória (PCR). Conselho Federal de Enfermagem, Brasília, DF, 2022.
CORREA, F. S., CHEVONIK, I. E., BRANDT, G. P., & BUCCO, M. Defibrillation by prehospital care nurses: evaluation of a training program. Electronic Journal Health Collection,v. 25, n. 5, p. e20237-e20237, 2025.
COSTA, A. J. S. D., CÂMARA, G., NOGUEIRA, P. J., & HENRIQUES, M. A. P. Nursing and the Sustainable Development Goals. Latin American Journal of Nursing, v. 31, p. e4037, 2023.
COSTA, D. C., DE SOUZA, J. A. P., DE SOUZA SILVA, M., DA SILVA, E. K. S., & DOS SANTOS SOUZA, M. C. Do-not-resuscitate (DNR) decisions in patients receiving palliative care: an integrative review. Academic Highlights Journal, v. 17, n. 3, 2025
COSTA, M. E. M., RODRIGUES, A. J., NAVES, H., ROCHA, K. D. F. F., PARENTE, L. E. G., FERREIRA, W. A., SOUSA, F. G., SANTOS., E. P., BARBOSA, W. M. C., MOURA., J. V. L., DIAS., P. V., SILVAIRA, C. R. R., RESQUE, R. F. C., JUNIOR, W. P. C., MARTINS, L. H. J., MARTINS, L. J., QUARIGUASI, P. G., QUARIGUASI, L. C. A. S. & MIRANDA, W. L. Use of rapid response protocols in the care of polytrauma patients: a literary review. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 9, p. 237253, 2024.
COUTINHO DA COSTA, J., PINHEIRO DE FRANÇA, L. I., LIMA DE OLIVEIRA, L. M., & SA BEZERRA GUERREIRO, T. The nurse’s contribution in cardiopulmonary arrest in the context of urgency and emergency in an in-hospital setting. Foco Magazine (Interdisciplinary Studies Journal), v. 17, n. 10, 2024.
CUNHA, K. P., NADAS, G. B., CERETTA, L. B., TOMASI, C. D., & TUON, L. Characterization of SAMU in Santa Catarina. Santa Catarina Medical Archives, v. 50, n. 2, p. 02-14, 2021.
CUNHA, V. P. D. Management of care by the multidisciplinary team for oncology patients in an intensive care unit. 2021.
D DOS SANTOS, A. C., CORREA, A. B., PEREIRA, D. L., PEREIRA, J. C. T., DE JESUS, L. C., DE ALMEIDA, S. R., & DE LEMOS, I. A.The nurse’s role in the care approach during cardiorespiratory arrest: training and updating in emergency and urgent care services. Contemporary Journal, v. 5, n. 8, p. e8608-e8608, 2025.
DA CONCEIÇÃO LUCENA, AT, DE SANT ANNA, AN, DE FREITAS, AH, DOS SANTOS LIMA, LM, & LIMA, DM. Cardiopulmonary resuscitation in pediatrics and neonatology: the evolution of care throughout history. Research, Society and Development, v. 11, n. 14, p. e308111436313-e308111436313, 2022.
DA COSTA JUNIOR, V. A., BRANCO, A. L. G. C., CAVALCANTI, A. L. M., BARROS, B. S., VASCONCELOS, D. M., DA SILVA NEGREIROS, F., & TEIXEIRA, L. N. A. The use of vasoactive drugs in the management of shock: a literature review. Research, Society and Development, v. 11, n. 10, p. e149111032453-e149111032453, 2022.
DA COSTA, J. C., DE FRANÇA, L. I. P., DE OLIVEIRA, L. M. L., & GUERREIRO, T. S. B. A. Nurses’ contribution to cardiorespiratory arrest in the context of urgency and emergency in the in-hospital environment. Foco magazine, v. 17, n. 10, p. e6618-e6618, 2024.
DA COSTA, L. V., LORDÃO, A. V., DA SILVA JÚNIOR, S. V., DA SILVA JÚNIOR, J. G., DE ARAÚJO, R. M. S. B., & DE LIMA, V. A. Care line for cardiorespiratory arrest in an adult intensive care unit: nurses’ role. International journal of Nursing Didactics, v. 13, n. 04, p. 06-14, 2023.
DA SILVA BEZERRA, J., SECATI, F., & MELO, A. G. . Difficulty in interpreting electrocardiograms by nurses. Journal of Faculties of Knowledge, v. 6, n. 13, p. 944-951, 2021.
DA SILVA COSTA, A. V. G., MOREIRA, V. G., SOUSA, R. C., LIMA, L. D. S. M., SILVA, Y., BATISTA, A. M., SANTOS, M. E., MEIRELES, M. S., SANTOS, L. V. B., & DA SILVA SOUZA, V. Basic life support: nursing students’ knowledge about the protocol for care in cardiorespiratory arrest. Interference: a journal of audio culture, v. 11, n. 2, p. 816-834, 2025.
DA SILVA DUARTE, A. C., CHÍCHARO, S. C. R., DA SILVA, K. C. F., VIANNA, T. A., DE OLIVEIRA, R. L., & DE SANTANA, W. K. F. An analysis of the last 20 years of American Heart Association protocols: What has changed in Basic Life Support?. Research, Society and Development, v. 10, n. 5, p. e5710514607-e5710514607, 2021.
DA SILVA FERREIRA, W., & FERREIRA, M. E. D. Nursing Team Knowledge of Patients with Cardiac Arrest (CPA) in the In-Hospital Environment. Cognition is scientific journal, v. 7, n. 2, p. e436-e436, 2024.
DA SILVA GOULART, M. G., LIMA, G. R., & DIAS, K. B. The nurse as a facilitating agent in improving basic life support. Health and Development Journal, v. 19, n. 31, p. 16-25, 2025.
DA SILVA OLIVEIRA, A. D., AZEVEDO, A. C. O., CARVALHO, É. V. M., SALES, I. C., & CORDEIRO, E. C. O. Use of Automated External Defibrillator (AED) in public places: Experience report. Interdisciplinary Journal, v. 17, n. 2, 2024.
DA SILVA OLIVEIRA, S., FERRAZ, M. O. A., BARATA, R. S., PITZER, C. M. T., DOS ANJO, K. F., SANTA ROSA, D. D. O., & LÍRIO, L. K. S. Ethical problems experienced by nurses in mobile pre-hospital care. REME- Minas Gerais Nursing Journal, v. 29, 2025.
DA SILVA PRADO, J. N.; DA SILVA, J. K. Extracurricular internship at SAMU (Emergency Medical Service): a potential tool in the training of nursing students. With Science Magazine, a multidisciplinary journal., v. 8, n. 12, p. e8122305-e8122305, 2023.
DA SILVA VARÃO, F., RIBEIRO, A. C. M., SAMPAIO, L. P., JÚNIOR, S. P. D. L. V., PINOTTI, M. L. A., MORAIS, A. V. N., Costa, L. S., Borba, W., Soares, G. P. S., Figueiredo, B. A. S., Sanches, I. M. O., Morais, I. C., Cardoso, C. D. L., & SILVA, L. M. The importance of cardiopulmonary resuscitation in pre-hospital care. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 2, p. 1612-1623, 2024.
DA SILVA, B. K. M., TASSARA, K. R., ANSALONI, L. V. S., DE MORAES, P. H. A., DE OLIVEIRA, R. A., & DA SILVA MATIAS, P. R. Knowledge about basic life support: an integrative review. Brazilian Journal of Development, v. 6, n. 9, p. 72021-72039, 2020.
DA SILVA, B. L., STELLA, C. R., MILANEZ, G. A., MACHADO, J. P., PEDERSOLI, C. E., & DEGANI, G. C. Airway management in the polytraumatized patient: an integrative review for nursing care. Interdisciplinary Journal of Health and Education, v. 5, n. 1, p. 245-261, 2024
DA SILVA, C. J., & DOS SANTOS MAIA, L. F. Hypothermia in patients after cardiopulmonary arrest in the intensive care unit. Recien: Scientific Journal of Nursing, v.12, n. 39, 2022.
DA SILVA, C. L. B., BLANCO, O. K. A., MACHADO, H. M. B., & GONDIM, D. A. D. The role of the nurse in prehospital care. Pey Këyo Multidisciplinary Scientific Journal ISSN 2525-8508, v. 8, n. 1, p. 66-85, 2022.
DA SILVA, D. G., DE SOUZA, C. J., SILVINO, Z. R., CORTES, A. L. B., & CASIMIRO, C. F. Management practices of nurses in mobile emergency medical services: an experience report. Electronic Journal Health Collection, v. 25, n. 5, p. e20471-e20471, 2025.
DA SILVA, E. B.; DA SILVA, J. P. M. Challenges and disparities in nurses’ response to cardiopulmonary arrest: a comprehensive analysis of practices and training in the hospital setting. JRG Journal of Academic Studies, v. 6, n. 13, p. 2448-2458, 2023.
DA SILVA, L. C., DE LIMA, F., ORTONI, G. E., ALMEIDA, J. B. M., DO AMARAL CARVALHO, J. M., DOS REIS, L. F. E. P., & PONTES, M. T. G. Integrated strategies and pre-hospital learning for optimizing stroke care pathways in the emergency network: a literature review. Europub Journal of Health Research, v. 6, n. 2, p. e5724-e5724, 2025.
DA SILVA, L. F. X., MORAIS FILHO, L. A., DE SOUZA, T. A., DE MEDEIROS, N. T. A. C., DE MATOS, J. H. F., SILVA, J. D. A., BARBOSA, Y. M. M., NASCIMENTO, A. K. F., CAMARGO, S. R. V., & DA SILVA FERREIRA, J. N. Knowledge of health science students regarding basic life support in cardiorespiratory arrest. Research, Society and Development, v. 10, n. 7, p. e21310715277-e21310715277, 2021.
DA SILVA, M. M., SILVÉRIO, J. E., DE SOUZA, A. C., DE LIRA SILA, M., & BRAGA, T. R. O. The importance of the nurse in performing quality CPR in pre-hospital care: a literature review. Ibero-American Journal of Humanities, Sciences and Education, v. 11, n. 10, p. 3506-3515, 2025.
DA SILVA, M. V., MOTTA, A. L. C., DA SILVA PEREIRA, L. D. F., DOS REIS, F. J., & FRANCELINO, A. L. M. The role of the nursing team in the face of cardiorespiratory arrest in mobile prehospital care. Contemporary journal, v. 4, n. 10, p. e6317-e6317, 2024.
DANTAS, B. A. D. S., POLICARPO, B. B., FONSECA, L. A. L., GALDINO, K. T. M., MACEDO, M. R. B. D., & SENA, J. F. D. Neonatal resuscitation determined by conditions in newborns treated in intensive and intermediate. Care unit, p. 13517-13517, 2025.
DE ALMEIDA, L. R., DE MENEZES, V. B., DE FARIAS, H. D. B., SOARES, M. H., DA SILVA, J. M., DA SILVA, A. R., & DE LIRA SOARES, H. Mobile prehospital care: evaluation of response time as a marker of survival in motorcycle trauma. Diversitas Journal, v. 5, n. 4, p. 2820-2838, 2020.
DE ALMEIDA, R. B., & ÁLVARES, A. D. C. M. Nursing care in mobile emergency medical services (SAMU): a literature review. Journal of Scientific Initiation and Extension, v. 2, n. 4, p. 196-207, 2019.
DE ALVARENGA, J. M. C., GOMES, A., SANTOS, A. B. D. S. C., DE MENEZES MENEGACE, D., SPOSITO, R. A., DE SOUZA FREITAS, L., VICTORETTI, I. A., SOUZA E SILVA, D., SANTOS, P. P. SOUSA, J. L., MARINHO, M. E. C. S., & DE SOUZA, J. A. S. Childhood drowning prevention: Essential strategies and the application of the chain of survival. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 1, p. 307-318, 2025.
DE ARAGÃO, I. P. B., DOS SANTOS, S. C. M., DOS ANJOS, I. L. P. B., JUNIOR, J. C. D. S. C., DE ARAGÃO, A. A. B., & NETO, A. R. B. Impacts of the Covid-19 pandemic on medical students’ knowledge of prehospital cardiopulmonary resuscitation. Mosaico Journal, v. 15, n. 1, p. 28-39, 2024.
DE ARAGÃO, I. P. B., DOS SANTOS, S. C. M., DOS ANJOS, I. L. P. B., JUNIOR, J. C. D. S. C., DE ARAGÃO, A. A. B., & NETO, A. R. B. Impacts of the Covid-19 pandemic on prehospital cardiopulmonary resuscitation knowledge among medical students. Mosaico Journal, v. 15, n. 1, p. 28-39, 2024.
DE ARAÚJO PINTO, A., DA SILVA SANTANA, M. R., NUNES, E. A. T., BARBOSA, K. T. F. F., XAVIER, A. T. T., DA SILVEIRA, M. M. B. M., & CABRAL, J. V. B. Knowledge of nursing students about the electrocardiogram. Nursing Brazil, v. 23, n. 2, p. 1623-1632, 2024.
DE ARAÚJO PORTO, V., DOS SANTOS, R. D. C., DA COSTA, M. F., MARQUES, G. Z., DA SILVA, M. B. S., DE FREITAS FERREIRA, F., & DA SILVA, D. N. Pediatric emergencies: multidisciplinary care. Advanced Studies on Health and Nature,v. 5, 2023.
DE ASSIS, A. C. P., DE OLIVEIRA NERY, A. P., DE OLIVEIRA NERY, M. L., & VILELA, R. D. C. B. D. Guidelines and Applications of Pediatric Advanced Life Support (PALS): Adaptations, Training, and Challenges. Journal of Advanced Clinical Implementation and Applied Medical Innovations (ISSN 3085-8348), v. 2, n. 02, p. 21-41, 2025.
DE AZEVEDO FILHO, E. R., GOMES, P. R. R., DE ARAÚJO, R. C. G., DE QUEIROZ, L. J., DA SILVA LOPES, A. C., & DE SOUZA SOARES, J. Emergency motorcyclist: a reflection of the daily challenges in pre-hospital care. Review, v. 11, n. 4, p. 723-734, 2022.
DE AZEVEDO, C. R. F., & DE MEDEIROS, J. A. Evolution in the Training of Facilitators for Continuing Education by the Continuing Education Center of SAMU 192 Regional Fortaleza. Chronos Urgência Magazine. v. 1, n. 1, p. e1121. 10-e1121. 10, 2021.
DE BARROS PRETTI, M., CAMPOS, S. B., PERUCHI, L. S., PRANDO, C. B., & VIEIRA, L. F. The influence of demographic profile on the outcome of chest pain in patients treated by SAMU in ES. Brazilian Journal of Health Review, v. 8, n. 1, p. e77968-e77968, 2025.
DE BARROS, L. C., DUARTE, S. K. A., OLIVEIRA, J. V. L., PINTO, H. P., VIEIRA, L. F., BARBOSA, R. R., .NETO, C. D., & SOGAME, L. C. M. Factors associated with mortality of patients with acute coronary syndrome who received prehospital care in the emergency medical service. Aracê, v. 7, n. 3, p. 15007-15022, 2025.
DE BESSA, P. H. C., GANDOLFO, C. P., DIAS, E. C., MOISÉS, M. C. B., VALENTIN, I. P. S., DE SOUSA LIMA, E. G. J., & DOS SANTOS, M. V. F. Level of knowledge of basic life support: from layperson to healthcare professional. An integrative review. Research, Society and Development, v. 12, n. 8, p. e15712842987-e15712842987, 2023.
DE BRITO, R. R., MILKEVIECZ, L., DOS SANTOS, L. B., LOPES, R. M., CUNHA, S. R. C., SERMIDI, M. P., RUBERT, A. L., & BASSON, J. C. F. The importance of cardiopulmonary resuscitation in the outcome of drowning. Contemporary Journal, v. 4, n. 9, p. e5862-e5862, 2024.
DE CAMARGO BENDINELLI, P., & HANGAI, R. K. Strategies for promoting patient safety in pediatric intensive care units: an integrative review. Journal of Health Administration, v. 24, n. 95, 2024.
DE CAMARGOS ROSA, G. F., SANTOS, J. R. D. O. G., & ZIMMER, L. D. M. J. Highperformance teams in cardiopulmonary resuscitation: can the use of identification badges help? LAJEC-Latin American Journal of Emergency Care, v. 3, n. 1, p. e23002-e23002, 2023.
DE CÁSSIA BITENCOURT, A., & RENNÓ, G. M. Basic life support in primary health care: an integrative literature review. Journal of Nursing and Health Care, v. 12, n. 1, 2023.
DE FARIAS, I. S. A., PINTO, L. V. D., DA COSTA, R. D. S., CHAGAS, T. A., SERRA, J. L., DE SOUZA, M. E. C. R., ARAUJO, R. L., ARAÚJO, R. S., SANTOS, A. B. A. S., ZANDIM, J. C. L., MEIRA., M. J., PORTUGAL., R. J., & TEIXEIRA, L. B. Knowledge of nursing professionals regarding cardiorespiratory arrest in emergency rooms. Research, Society and Development, v. 10, n. 16, p. e499101622373-e499101622373, 2021.
DE FARIAS, W. S., DA SILVA FILHO, M. A., DA SILVA, N. D. C., LEAL, S. M. O. S., SANTOS, K. R. M., DA SILVA BRITO, M. I. B., & FARIAS, S. Thoracic decompression performed by a pre-hospital care nurse using needle decompression. Brazilian Journal of Health Review, v. 7, n. 1, p. 4773-4781, 2024.
DE FRANÇA, T. C. M. L., & DA SILVA TENÓRIO, H. A. Airway management using a laryngeal mask by nurses in emergency situations: an integrative review. Brazilian Journal of Health Review, v. 6, n. 1, p. 886-897, 2023.
DE JESUS, R. S., PFAFFENBACH, G., & GOMES, L. E. M. Nursing management in urgency and emergency care. Electronic Journal Health Collection, v. 24, n. 1, p. e14485e14485, 2024.
DE LIMA NETO, A. V., LIMA DE MELO, V., VIEIRA DANTAS, D., & FERNANDES COSTA, I. K. Postoperative complications of cardiac surgery in adult patients: a comprehensive review. Science and nursing, v. 27, 2021.
DE LIMA TORRES, V., DICK, N. R. M., KOLLET, J. M. S., & PINTO, J. N. Knowledge and application of cardiopulmonary resuscitation protocols by primary healthcare nurses. Perspective Magazine: Science and Health, v. 8, n. 2, 2023.
DE LIMA, L., SANTOS, C. F. D., COUTINHO, F. M., SANTOS, H. F. D., SOUZA, J. S., & SANTOS, J. B. D. The importance of the nurse in the implementation of the CPR protocol. In: Nursing in focus: education, competencies and advanced practices – v 2,. p. 99-106, 2024.
DE LIMA, M. A. G., BRANDÃO, F. J. M., AGUIAR, M. D. F. A., DA SILVA GOMES, A. A., PAIVA, F. D. A. F., MENEZES, R. S. P., & DE MELO, T. S. Analysis of the knowledge of nurses working in inpatient units regarding cardiorespiratory arrest. Research, Society and Development, v. 14, n. 8, p. e7614849428-e7614849428, 2025.
DE LIMA, M. B., DA SILVA PONTES, J., & RAMOS, R. R. The impact of early, highquality CPR in adults and older adults: an integrative review. Biosciences and Health, v. 2, p. 1-10, 2024.
DE LIMA, V. M., VERÍSSIMO, R. C. S. S., DOS SANTOS, A. A. P., CALHEIROS, M. D. M. F., & SANTOS, J. A. M. Patient care during orotracheal intubation: the nurse’s practice. Principia Journal, n. 56, p. 64-71, 2021.
DE MATTOS OLIVEIRA, C. W., HADDAD, L. L., MILFONT, K. L., BARRAZA, J. P. P., BEZERRA, A. R. S., DE LIMA, M. H. V., & GONÇALVES, A. G. T. Challenges and strategies in emergency intubation: clinical and technical approaches to ensure airway safety. Educational Handbook, v. 21, n. 13, p. e12942-e12942, 2024.
DE MELO, R. A., FERNANDES, F. E. C. V., COQUEIRO, L. S. R., DE MELO, D. C., & CARVALHO, M. C. Communication and obstacles in the work process of emergency and urgent care teams. Nursing Today in Dermatology Journal, v. 97, n. 4, p. e023187e023187, 2023.
DE MIRANDA, R. B., VIANELLO, M. A., DE OLIVEIRA, G. M., LINCOPAN, N., & QUEIROZ, I. T. Fungemia caused by Kodamaea ohmeri in a patient with severe COVID-19 – case report. The Brazilian Journal of Infectious Diseases, v. 27, p. 103294, 2023.
DE MORAIS SILVA, A., SANTOS, L. D. L. Q., CARVALHO, W. L., BOTENTUIT, T. N. A., SOUSA, J. A. F., PITTA, B. C., & GOMES, N. H. Resuscitation of newborns in delivery rooms and their outcomes: a review study. Brazilian Journals. Scientific Research, v. 3, n. 2, p. 38-45, 2024.
DE OLIVEIRA MARQUES, T., DE MELO, L. D., TAROCO, F. E., DE LIMA DUARTE, R. M., & DE LIMA, H. D. Mobile Emergency Care Services (SAMU): an integrative review. Research, Society and Development, v. 10, n. 2, p. e38310212522-e38310212522, 2021.
DE OLIVEIRA SANTOS, W. H., DE OLIVEIRA, R. F., CARVALHO, E. A. C., DE PINHO, L. A., DALTRO, A. C. V., DA CRUZ, N. R. S., & BUSS, A. P. T. Nursing care for patients in cardiorespiratory arrest: an integrative review study. Brazilian Journal of Implantology and Health Sciences, v. 5, n. 4, p. 1683-1694, 2023.
DE OLIVEIRA XAVIER, B., DE ALMEIDA MARQUES, A., & DE LEMOS, I. A. Nurses’ Protagonism in Interventions in Cardiopulmonary Arrest Situations. Research, Society and Development, v. 14, n. 8, p. e5214849378-e5214849378, 2025.
DE OLIVEIRA, A. B. The role of the nurse in cases of cardiorespiratory arrest: an integrative literature review. Research, Society and Development, v. 11, n. 12, p. e582111235159e582111235159, 2022.
DE OLIVEIRA, M. G., BASTOS, F. V., DE SOUSA, G. C. S., MOITA, S. M., DE AZEVEDO, C. R. F., & VASQUES, P. H. D. A Comparative analysis of care for suspected acute myocardial infarction and stroke in pre-hospital care. LAJEC-Latin American Journal of Emergency Care, v. 5, n. 1, 2025.
DE OLIVEIRA, M. V. Continuing education – an essential component for excellence in emergency nursing care: A narrative review. Research, Society and Development, v. 14, n. 4, p. e0914448503-e0914448503, 2025.
DE OLIVEIRA, W. A., CAPELOA, C. N., OCON, C. A., DA CUNHA, M. F., LAZZARESCHI, L., FILONI, E., PALINSKI, J. R., PALINSKI, J. R., BARBOSA, M. H., LOPES, M. & OLIVEIRA, R. D. R. S. The evolution and implementation of the mobile emergency care service (SAMU) in Brazil. Observatory of the Latin American Economy, v. 22, n. 8, p. e6465-e6465, 2024
DE PAULO, I. J. M., RODRIGUES, E. F. S., DA SILVA, I. G., MOREIRA, L. D. F. S., DE PAULA SILVA, T., DA SILVA SOUZA, Y., & SILVA, D. W. R. Nursing students’ knowledge about cardiopulmonary resuscitation: an integrative review. Uningá Journal, v. 58, p. eUJ3252-eUJ3252, 2021.
DE SA CÂMARA, S. B., DE QUEIROZ, M. E. M., CÂMARA, O. F., & DUARTE, E. A. A. Initial care profile of the mobile emergency care service (SAMU) for polytrauma patients directed to a hospital in Acre, between 2020 and 2022. Electronic Journal Health Collection, v. 24, n. 11, p. e17599-e17599, 2024.
DE SOUSA FERREIRA, T. D., DA SILVA, M. A. C. L., FERNANDES, F., CAVALCANTE, L. L. P., DE OLIVEIRA, M. A. C., DE LIMA, C. B. V., & DE SOUSA, R. V. The role of nurses in responding to cardiac emergencies and urgencies in the SAMU (Brazilian Mobile Emergency Medical Service): an integrative literature review. IberoAmerican Journal of Humanities, Sciences and Education. v. 11, n. 4, p. 3860-3872, 2025.
DE SOUSA FERREIRA, T. D., DA SILVA, M. A. C. L., FERNANDES, F., CAVALCANTE, L. L. P., DE OLIVEIRA, M. A. C., DE LIMA, C. B. V., & DE SOUSA, R. V. The role of nurses in responding to cardiac emergencies and urgencies in the SAMU (Emergency Medical Service): an integrative literature review. Ibero-American Journal of Humanities, Sciences and Education, v. 11, n. 4, p. 3860-3872, 2025.
DE SOUSA, G. L. The inclusion of physiotherapy in mobile emergency medical services (SAMU). Multidisciplinary Journal of Health., v. 2, n. 4, p. 234-234, 2021.
DE SOUZA LIMA, R. M., FELIX, J. V. C., MIRANDA, F. M. D. A., MEIER, M. J., & DE ALMEIDA CRUZ, E. D. Realistic multi-victim simulation in a hospital setting with nursing students. Electronic Journal Health Collection, v. 24, n. 10, p. e17804-e17804, 2024.
DE SOUZA MARQUES, J. B., DE ASSIS, L. R., DA SILVA, S. A., DE OLIVEIRA, A. V., DE OLIVEIRA, C. F. P., DE LAFFITTE, E. A. D. S., & DA ROCHA PINTO, M. D. F. Ultrasound in pre-hospital care: the role of the nurse in decision-making in the management of trauma victims. Observatory of the Latin American economy, v. 23, n. 6, p. e10152e10152, 2025.
DE SOUZA, A. D., DE LIRA SILVA, M., & DE OLIVEIRA NÓBREGA, R. Safety in medication administration: practices and challenges faced by nursing professionals. IberoAmerican Journal of Humanities, Sciences and Education, v. 11, n. 6, p. 3422-3434, 2025.
DE SOUZA, C. E. A., DA SILVA LIMA, H. C. A., FARIAS, A. F. D. C., DE SENA CERQUEIRA, T., DE OLIVEIRA CORDEIRO, A., DA SILVA NOGUEIRA, N., FROTA, M. E. S., NASCIMENTO, N. G., JÚNIOR, F. M. S., OLIVEIRA, G. R., COUTINHO, J. H. B. S., FILHO, J. I. S. S., MACIANO, J. F. S., TEIXEIRA, R. O., & DE FIGUEIREDO GONÇALVES, M. Post-cardiac arrest patient care. Advanced Studies on Health and Nature, v. 4, p. 165-178, 2022.
DE VASCONCELOS TEIXEIRA, M., DE SOUZA, M. D. P. G., DE MELO, L. M. G., BARBOSA, V. G. B., & DOS SANTOS, E. L. Therapeutic hypothermia induced in the intensive care unit: an integrative literature review. JRG Journal of Academic Studies, v. 7, n. 15, p. e151423-e151423, 2024.
DEGANI, G. C., DE OLIVEIRA, G. C., VIOLA, L. F., DE SOUSA COSTA, S., MASELLA, C. A., & SIMÕES, I. I. Impact and recommendations for the use of defibrillators in cardiorespiratory arrest by nurses: an integrative review. Interdisciplinary Journal of Health and Education, v. 6, n. 1, p. 211-231, 2025.
DERENZO, N., DE MIRANDA, D. J. C., DA SILVA, S. L. P., NEVES, I. F., MENDONÇA, R. R., SALVADOR, D. L. V. F., CHRISTINELLI, H. C. B. & STEVANATO, K. P. Profile of emergency care at a base in northwestern Paraná. Research, Society and Development, v. 10, n. 5, p. e14010514859-e14010514859, 2021.
DIAS, B. F., SALBEGO, J. E. A., COSTA, N. P. D., DE MELO RIBEIRO, B., SAVIO, R. W., MICHELINI, A. C. L., & VENTURA, A. F. G. Challenges of cardiopulmonary arrest in pre-hospital settings: a literature review. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 8, p. 642-648, 2024.
DINIZ, L. N., NETO, S. D. C. C., JAPIASSÚ, V. B., & DA SILVA, R. M. Regulation for SAMU based on a fictitious clinical case – experience of medical students. REVOLUA Magazine, v. 2, n. 2, p. 320-325, 2023.
DO CARMO MENEGAZI, J., DE LIMA TRINDADEI, L., & DOS SANTOSII, J. L. G. Entrepreneurship in nursing: contribution to the sustainable development goal of Health and Well-being. Rev enferm UERJ, 2021.
DO CARMO SANTOS, J. The work process of nurses in mobile pre-hospital care. ESP Notebooks, v. 15, n. 1, p. 49-62, 2021.
DO CARMO SANTOS, J., PEQUENO, A. M. C., JÚNIOR, A. G. M., & DA SILVA NEGREIROS, F. D. The work process of nurses in mobile pre-hospital care. ESP Notebooks, v. 15, n. 1, p. 49-62, 2021.
DO MONTE, B. F., SILVA, A. C. G., DE AGUIAR, V. N. O., DE SÁ JUNIOR, J. X., DE CARVALHO JUNIOR, J. F., DE ARAÚJO, R., LIMEIRA, B. S., & LIMA, M. A. B. Nurses’ perceptions of advanced nursing practices and intermediate life support. Observatory of the Latin American Economy, v. 22, n. 10, p. e7222-e7222, 2024
DO NASCIMENTO SARAIVA, G. B., MARQUES, L. R., ALMEIDA, L. C. P., & BARROS, M. M. A. Nurses’ perception of mobile prehospital care related to intermediate life support (IVS). Electronic Journal of Health Archives, v. 13, n. 1, p. e5581-e5581, 2021.
DO NASCIMENTO, B. T. S., DE LEMOS SCHULER, M. F., DO NASCIMENTO, A. C. F., DE ARAUJO COSTA, Y. F., MELO, E. A., MESQUITA, T. B., & DO NASCIMENTO, M. S. Management of cardiopulmonary resuscitation in the neonate. Brazilian Journal of Implantology and Health Sciences, v. 5, n. 4, p. 1089-1100, 2023.
DO NASCIMENTO, G. L. S., DE AGUIAR, F. B., DE OLIVEIRA, H. B. A., DE OLIVEIRA, H. M., CONCEIÇÃO, J. C. N., DE CAMPOS MADIA, H., FIORAMONTE, G. L. N., DORETO, M. X., SILVA, B. D., CRUZ, A. N., MOTA, V. G., CASTELAN, L. A., REIS, W., PEREIRA, Z. B., & MACEDO, L. S. Effectiveness of Cardiopulmonary Resuscitation in Emergency Settings: Updates and Best Practices in Advanced Life Support. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 2, p. 60-71, 2025.
DO NASCIMENTO, G. R. M. S., DE CARVALHO, A. E. L., SILVEIRA, C. D. L. S., DE ARAÚJO, A. M., ROGES, A. L., & DE FREITAS COMBE, M. E. Contributions to safe nursing practices in pre-hospital care: a systematic review: systematic review”. Health (Santa Maria), v. 51, p. e85399-e85399, 2025.
DO NASCIMENTO, J. B., DE OLIVEIRA, D. R. R., DE SOUZA SANTOS, S., & GUTIERRES, L. L. B. The importance of basic life support training in the face of cardiorespiratory arrest for primary healthcare nurses: an integrative review. Observatory of the Latin American Economy, v. 22, n. 9, p. e6626-e6626, 2024.
DOS REIS, G. R., DA SILVA, G. L. G., ALMEIDA, H. W. S., RIBEIRO, J. R. L., CHAVES, D. D. F. F., DE OLIVEIRA, C. F. P., PEREIRA, D., & DA SILVA PEREIRA, R. M. The role of the nursing team in cardiopulmonary arrest: a literature review. Aracê, v. 7, n. 5, p. 2432924346, 2025.
DOS SANTOS CARVALHO, M., SENA, A. B., DE CARVALHO, A. O., ARCANJO, A. S., DE MELLO, B. M. M., DE LIMA, E. T. B., … & DO NASCIMENTO, V. M. S. .Effectiveness of Advanced Life Support Protocols in Pre-hospital Care of Cardiorespiratory Arrest: An Integrative Review. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 7, p. 2684-2698, 2024.
DOS SANTOS CLAUDIANO, M., LOPES, N. N. L., & FIORIN, B. H. Knowledge, Attitudes and Practices of Nurses in Cardiopulmonary Resuscitation: Development of an Instrument. Nursing Brazil, v. 23, n. 1, p. 1273-1285, 2024.
DOS SANTOS MOTA, R., DOS SANTOS, J. E., DE ALMEIDA, P. L. S., DE OLIVEIRA, E. R. L., SOUZA, A. L. M., & JUNIOR, A. S. C. Experience report – LATE in the mobile emergency medical service (SAMU) in 2019. Brazilian Journal of Health Review, v. 5, n. 4, p. 12595-12605, 2022.
DOS SANTOS PEREIRA, E.; DA SILVA LOPES, L.; DOS SANTOS PEREIRA, E. Pharmacological iatrogenesis caused by medications used during Cardiopulmonary Arrest: a narrative review. Electronic Journal Health Collection, v. 13, n. 2, p. e2818-e2818, 2021.
DOS SANTOS, A. C., CORREA, A. B., PEREIRA, D. L., PEREIRA, J. C. T., DE JESUS, L. C., DE ALMEIDA, S. R., & DE LEMOS, I. A. Nurses in the care approach to cardiorespiratory arrest: training and updating in emergency services. Contemporary Journal, v. 5, n. 8, p. e8608-e8608, 2025.
DOS SANTOS, J. B., & COSTA, C. R. B. Cardiorespiratory arrest: post-resuscitation care after return of spontaneous circulation. Research, Society and Development, v. 11, n. 13, p. e167111335251-e167111335251, 2022.
DOS SANTOS, L. B., FREITAS, A. S., DE CERQUEIRA, D. C. G., & DOS REIS, L. A. Nursing care in the face of cardiorespiratory arrest in the Emergency Unit: A narrative review of the literature. Research, Society and Development, v. 13, n. 10, p. e118131047079e118131047079, 2024.
DOS SANTOS, M. A. C., DOS SANTOS, S. C. M., DOS SANTOS, P. A. S., DOS SANTOS SILVA, M. A., TRAJANO, E. T. L., & DE ARAGÃO, I. P. B. Training in Out-of-Hospital Cardiopulmonary Resuscitation. Comparison Between Students in the Humanities and Health Areas. Mosaico Magazine, v. 15, n. 1, p. 131-146, 2024.
DOS SANTOS, M. S., DE JESUS, V. M. C. C., DE ANDRADE, A. F. S. M., DOS SANTOS, J., & DE OLIVEIRA, M. D. C. The nurse’s role in cardiopulmonary resuscitation in hospitalized adults: an integrative review. Bahian Journal of Public Health, v. 48, n. 4, 2024.
DOS SANTOS, T. D. V., DOS SANTOS SILVA, J. L., XAVIER, R. A. L., DO NASCIMENTO, A. S., JOBIM, M. L. A., DA SILVA, J. P. M., & DOS SANTOS SIMÕES, T. Evolution of prehospital care practice in Brazil: a historical synthesis. JRG Journal of Academic Studies, v. 6, n. 13, p. 1082-1090, 2023.
DOS SANTOS-RODRIGUES, R., MONTEIRO-BATISTA, C., & LAUDARES-KAWAGUCHI, I. A. Analysis of incidents carried out by the Emergency Medical Service (SAMU/DF). Scientific Journal of Care, p. 23-33, 2024.
DUTRA, G. G., DE SIQUEIRA, H. C. H., FLORES, R. G., BICK, M. A., DE ÁVILA, L. F. G. E., & DE PAULA, S. F. Regional continuing education center in emergency care services: nurses’ perceptions. Cuadernos de Educación y Desarrollo, v. 16, n. 3, p. e3552-e3552, 2024.
ELMER, J., ATKINS, DL, DAYA, MR, DEL RIOS, M., FRY, JT, HENDERSON, CM, & IDRIS, AH. Nurses’ attitudes and confidence towards defibrillation and cardiopulmonary resuscitation: a cross-sectional study in Hong Kong. International Emergency Nursing, v.19, n. 4, p. 220–228, 2011.
EUROPEAN RESUSCITATION COUNCIL. ERC Guidelines on Cardiopulmonary Resuscitation 2025. Niel, Belgium: European Resuscitation Council VZW; 2025.
FEDERAL COUNCIL OF NURSING (COFEN). Resolution No. 564, of November 6, 2017. Approves the Code of Ethics for Nursing Professionals. Official Gazette of the Union, Brasília, DF, November 6, 2017.
FEDERAL COUNCIL OF NURSING (COFEN). Resolution No. 704, of July 19, 2022. Regulates the performance of nursing professionals in the use of defibrillation equipment in the care of individuals in cardiorespiratory arrest (CRA). Official Gazette of the Union, Brasília, DF, July 22, 2022.
FELIPE, T. F., CASIMIRO, M. R. A., DE SOUZA, A. C., & OLIVEIRA, G. S. The importance of the nurse in the execution and interpretation of the electrocardiogram for quality care. Ibero-American Journal of Humanities, Sciences and Education, v. 11, n. 5, p. 3289-3299, 2025.
FILIPPIN, M. L. D., & LISIESKI, N. Prehospital care: factors influencing nursing work. In: Nursing: Research that Transforms Practice. Editora Científica Digital, 2024. p. 62-77.
FINN, J. Teaching basic life support to nurses: the effect of clinical experience on learning. Resuscitation, v. 32, n. 1, p. 45–51, 1996.
FORASTIERI FILHO, H. L. A., DE ARAUJO, C. M. F., JUNIOR, A. D. S. M., & FORASTIERI, H. L. C. Response time at SAMU-192 and its implications. UniFOA Notebooks, v. 17, n. 49, p. 173-183, 2022.
FORMOSO MACHADO, K. L., BERNARDO DA SILVA, M. R., SOARES DE SOUZA, D.R., DA SILVA ROCHA PRADO, L., FERNANDES DOS SANTOS, M., DA CONCEIÇÃO SABINO, G., & DE ARAUJO, D. M. The role of the nurse in contemporary mobile prehospital care services: an integrative review. Public Health, v. 11, n. 65, 2021.
FRISANCO, F. M., BARBIERI, M. R. B., GORLA, B. C., AFONSO, M. G., ASSALIN, A. C. B., DE SOUZA ORLANDI, F., & GIRÃO, F. B. Competencies of nurses in the care of patients with Covid-19 on invasive mechanical ventilation in hospital settings: a scoping review. Research, Society and Development, v. 11, n. 12, p. e42111234107-e42111234107, 2022.
FRÓES, E. C. A., DA SILVA, H. A., BARBOSA, S. L., BRANDÃO, W. L., DE OLIVEIRA, J. N. A., DA ROCHA JUNIOR, W. R., SANTOS, P. G., ROCHA, R. M. B., DIAS., G. T., GONÇALVES, L. C. S., COSTA., A. N., MUNIZ, F. J., SCREMIN, M., MONTEIRO, S. C., ALENCAR, A. M., & MOTA, L. R. Profile of mobile emergency care in Brazil – literature analysis. Research, Society and Development, v. 11, n. 9, p. e47411925812-e47411925812, 2022.
GALÁN MORALES, A. E. Level of knowledge in CPR among nursing staff in the operating room area. Veracruz University. Faculty of Nursing, 2025.
GASPAR, C. L. I., & LIMA, R. A. Challenges faced by nurses in leading cardiopulmonary resuscitation in hospital settings: an integrative review. Remecs Journal – Multidisciplinary Journal of Scientific Studies in Health, p. 32-32, 2025.
GIL, A. B., BRITO, J. N. M., SILVA, N. M., DO NASCIMENTO LEITE, S. J., & BITENCOURT, A. L. S. Continuing Education in Cardiopulmonary Resuscitation as a qualifying strategy for Nursing – Reference Hospital of the Federal District. JRG Journal of Academic Studies, v. 8, n. 18, p. e181823-e181823, 2025.
GOGOLA, J., KISNER, E., MALGARIN, J. S., DE OLIVEIRA BELLANI, W. A. G., & DE SOUZA, J. M. Cardiopulmonary resuscitation by laypersons – techniques and auxiliary tools: an integrative review. Space for Health, v. 24, 2023.
GOMES, R. C., & GALINHA-DE, F. L. F. R. Nursing interventions for individuals with acute myocardial infarction after cardiopulmonary arrest: an integrative literature review. Brazilian Journal of Health Review, v. 8, n. 1, p. e77726-e77726, 2025.
GONÇALVES, D. S. B. Simulated Advanced Life Support Practice – Specialized Team Training. Polytechnic Institute of Castelo Branco, 2023.
GONÇALVES, M. S. The role of the nurse in mobile pre-hospital care: challenges. DELOS Magazine, v. 18, n. 63, p. e3871-e3871, 2025.
GUEDES, A. R., AMARO, A. Y. G., DE SOUZA, N. P., DE SOUZA LIMA, M., NASCIMENTO, Â. C. B., & NEVES, F. L. A. The importance of training nursing professionals in the face of cardiorespiratory arrest in adults. Facit Business and Technology Journal, v. 1, n. 26, 2021.
GUEDES, A. R., AMARO, A. Y. G., de SOUZA, N. P., de Souza Lima, M., NASCIMENTO, Â. C. B., & NEVES, F. L. A. The importance of training nursing professionals in responding to cardiorespiratory arrest in adults. Facit Business and Technology Journal, v. 1, n. 26, 2021.
GUEDES, J. P. P., FORTES, B. C. R., DE PAIVA, F. J. P., SCHIMDT, I. A., PINTO, L. B. S., VIEIRA, L. K., CUNHA, L. L., SETTE, T. E., DIAS, A. M. N., MENDES, N. B. E. S., & CORREA, C. R. Analysis of care provided to patients in cardiorespiratory arrest by SAMU. Brazilian Journal of Development, v. 8, n. 9, p. 63286-63297, 2022.
GUIMARÃES, H. P., TIMERMAN, S., RODRIGUES, R. D. R., CORRÊA, T. D., SCHUBERT, D. U. C., FREITAS, A. P., & LOPES, M. A. C. Q. Position statement on cardiopulmonary resuscitation for patients diagnosed with or suspected of having COVID-19 – 2020. Brazilian Archives of Cardiology,v. 114, n. 6, p. 1078-1087, 2020.
GUIMARÃES, L. N., FERREIRA, N. R., DE ALMEIDA RIBEIRO, G. M., SILVA, D. A., DE FONSECA, R. A., BARROS, L. A., LEMES, B. R. S., SILVA, J. C., ROCHA, C. F., LIMA, R. K. M., WESTRY, A. G. A., SILVA, J. C. & GONÇALVES, R. J. W. Multidisciplinary Care in CPA and Advances in Literature Review. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 7, p. 2475-2484, 2024.
HALEY, M. The role of nursing in the management of cardiorespiratory arrest. Academic Journal of Health and Education,v. 1, n. 02, 2023.
HERMILLY, M., MICHEL, F., HANOUZ, J., MACREZ, R., AUBRION, A., CLANET, R. Using the simple consensus method to create an aid tool for activating a helicopter service in SAMU 14. Santé Publique, v. 35, n. 5, p. 7-12, 2023.
HONORATO, P. F., NASCIMENTO, B. C., BARROS, A. J. F., NETO, L. E. F., DE OLIVEIRA, Y. P., TELES, M. S., TRAJANO, L. S., TOMAS, S. H., LIMA, B. C., SANTOS, S. B. C., ALVES, R. A., ARRUDA, A. L. A. S., & VENÂNCIO, D. O. The Impact of PreHospital Care on Reducing Mortality from Acute Myocardial Infarction: Time-Dependency and Rapid Intervention Strategies. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 3, p. 1532-1537, 2025.
IWAMI, T., KAWAMURA, T., HIRAIDE, A. Continuous improvements in chain of survival increased survival after out-of-hospital cardiac arrest. Circulation, 119(6), 728–734, 2009. JOSHI, A., SMITH, L., & BROWN, K. Effectiveness of rehabilitation interventions on the secondary consequences of surviving a cardiac arrest: a systematic review and meta-analysis. Resuscitation, v. 172, p. 1-15, 2022.
JUNIOR, E. P. T., & DE ARAÚJO, A. H. I. M. Nursing care in SAMU and its legal support: a bibliographic review. JRG Journal of Academic Studies, v. 6, n. 13, p. 2317-2332, 2023.
JÚNIOR, L. D. S. S., DE MELLO, M. E. R., ANGEL, D. J., & DA NÓBREGA DANTAS, M. F. Challenges faced by nursing professionals in pre-hospital care: an integrative review. Focus Magazine, v. 18, n. 3, p. e8036-e8036, 2025.
KESSLER, DO, LEMKE, DS, JANI, P., DEWAN, ML, MOORE-CLINGENPEEL, M., CHANG, TP, … & WOLFE, HA. Caregiver Characteristics Associated With Quality of Cardiac Compressions on an Adult Mannequin With Real-Time Visual Feedback: A Simulation-Based Multicenter Study. Resuscitation Plus, v. 5, p. 100078, 2021.
KINAMA, V. C., GABRIEL, C. V. R., AFONSO, C. D. J., SANHANGUE, C. F., GERMANO, C. H. J., MANUEL, C. D. P., & CHOLE, C. M. D. S. The role of nurses in cases of cardiorespiratory arrest (CRA) in Angola. Ibero-American Journal of Humanities, Sciences and Education, v. 9, n. 7, p. 1-14, 2023.
KUNZ, A.; GONÇALVES, C.; CAMPOS, K.; SOUZA, R.; SANTOS, A. Nurses’ perceptions regarding the use of the laryngeal mask in the in-hospital setting. Research, Society and Development, v. 11, n. 16, p. e380981604287, 2022.
KURTZ, B. E., & MARTINS, W. Analysis of care provided to patients in cardiorespiratory arrest by SAMU. Research, Society and Development, v. 11, n. 5, p. e58311528499e58311528499, 2022.
LANDA, J., & FERREIRA, A. M. G. B. Transferring Knowledge of Basic Life Support to Laypeople and Healthcare Professionals: an integrative review. Brazilian Multidisciplinary Journal, v. 23, n. 2Supl., p. 99-114, 2020.
LAPORTE, K. F., DE SOUZA, R. M., FARIA, M. F. G. C., DE SOUZA DOURADO, C., RAMOS, J. L. S., & LOUREIRO, R. J. Assessment of the importance of continuing education in basic life support for healthcare professionals. International of the Unified Network, 2021.
LEAL, L. B., PORTES, A. A. R., SAMPAIO, A. J. R., ANDRADE, A. B. P., & MENDES, M. V. A. Evidence-based practices and primary assessment in pre-hospital care: impact on survival in trauma cases. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 2, p. 280-291, 2025.
LIEBICH, M. V. B., LIEBICH, J. P. B., KAZAMA, A. T. R., & GRIEP, R. Assessment of the impact of implementing a pre-hospital care system on mortality from acute myocardial infarction in the 10th health region – Cascavel. Ibero-American Journal of Humanities, Sciences and Education, v. 9, n. 8, p. 2583-2590, 2023.
LIMA, B. D. D. S. D., MATOS, A. B. D. O. V., RABITO, L. B. F., GONÇALVES, T. L. P., FLÁVIO, G. G., & LEAL, E. S. Analysis of the response time indicator of the mobile emergency care service (SAMU). Nursing (Ed. bras., Impr.), p. 8318-8329, 2022.
LIMA, I. O., NUNES, L. M. C., de ARAÚJO, S. A., CHAGAS, D. R., & AMARO, A. Y. G. Basic life support in pediatrics: scientific evidence. Facit Business and Technology Journal, v. 1, n. 60, 2025.
LIMA, J. L. M. Nurses’ knowledge in interpreting electrocardiograms: an integrative literature review, 2021.
LOPES, A. P. O., & NOGUEIRA, G. B. The nurse’s knowledge and role in providing inhospital care to victims of cardiorespiratory arrest. Electronic Journal Health Collection,v. 13, n. 5, p. e7520-e7520, 2021.
LOPES, S. J. C., RAMOS, D. P., DOS SANTOS GOMES, D., LOPES, F. C., PONTES, F. G. A., DE SOUZA, J. B. N., SALES, M. L., & DE ARAÚJO, N. N. M. The importance of international patient safety goals in promoting safe and effective healthcare practices. Pedagogical Notebook, v. 22, n. 7, p. e16603-e16603, 2025.
LÓPEZ-HERCE, J., MANRIQUE, I., CALVO, C., RODRÍGUEZ, A., CARRILLO, Á., SEBASTIÁN, V., & DEL CASTILLO, J. New developments in pediatric cardiopulmonary resuscitation recommendations and development lines in Spain. In: Anales de Pediatría. Elsevier Doyma, p. 146. e1-146. e11, 2022.
LUDWIG, E. F. D. S. B., HADDAD, M. D. C. F. L., MOREIRA, M. Â. R., GAVIOLI, A., BARRETO, M. F. C., PEREIRA, M. C. A., MARTINS, E. A. P., & NOGUEIRA, L. D. S. Quality indicators of a Mobile Emergency Care Service. Paulista Nursing Journal, v. 38, p. eAPE00114, 2025.
M MITIDIERI, B., BERTOLIN, D., & GABRIEL, S. A. Review of protocols for the management of acute coronary syndrome and cardiorespiratory arrest: a comparative analysis between the guidelines of the American Heart Association and the Brazilian Ministry of Health. Corpus Hippocraticum Journal, v. 1, n. 1, 2025.
MACHADO, C. V., SALVADOR, F. G. F., & O’DWYER, G. Mobile Emergency Care Service: analysis of Brazilian policy. Journal of Public Health,v. 45, p. 519-528, 2011.
MALVESTIO, M. A. A., & SOUSA, R. M. C. D. Inequality in pre-hospital care in Brazil: analysis of the efficiency and sufficiency of SAMU 192 coverage. Science & Public Health, v. 27, n. 7, p. 2921-2934, 2022.
MALVESTIO, M. A. A.; SOUSA, R. M. C. Inequality in pre-hospital care in Brazil: analysis of the efficiency and sufficiency of SAMU 192 coverage. Science & Public Health, v. 27, n. 7, p. 2921-2934, 2022.
MARCELINO, B. F., DOS SANTOS, M. L. P., DE SENA, A. S. R., NUVENS, J. S., DA SILVA SANTOS, T., INÁCIO, T. S., ARAÚJO, S. G., VIDAL, E. C. F., SAMPAIO, L. R. L., & PINHEIRO, W. R. Nursing care in pre-hospital cardiorespiratory arrest situations. Electronic Journal of Health Archives,v. 25, n. 5, p. e20201-e20201, 2025.
MARCUSSI, V. M., HASHIMOTO, M. N., ZANUSSO-JUNIOR, G., FERREIRA, M. R. M. N., HIGA, T. T., LEMOS, M. M., FRASCISCO, M. C., & BITTENCOURT, M. R. Prehospital transfusion in air ambulance – assessment of patient survival. Hematology, transfusion, and cell therapy, v. 46, p. S828, 2024.
MARQUES, A., & RODRIGUES, A. Poster 13: Difficulties Faced by Nurses in Assisting with In-hospital Cardiorespiratory Arrest: a Research Project. II International Conference, p. 61, 2025.
MARQUES, S. F. A. Challenges of in-hospital resuscitation: Perception of difficulties faced by nurses in the inpatient ward and the in-hospital medical emergency team. 2025.
MARTINS, A. L. J., MIRANDA, W. D., SILVEIRA, F., & PAES-SOUSA, R. A Book 2030 and the Sustainable Development Goals (SDGs) as a strategy for equity in health and sustainable and healthy territories. Health in Debate, v. 48, p. e8828, 2024.
MARTINS, P. P. S., & PRADO, M. L. D. Nursing and pre-hospital care services: challenges and perspectives. Brazilian Journal of Nursing, v. 56, p. 71-75, 2003.]
MARTINS, R. C. C., SILVA, E. S., VICENTE, J. G., & MILANI, R. G. Students’ perceptions of health promotion in higher education and quality of life. Brazilian Journal of Health Promotion, v. 35, p. 11-11, 2022.
MASTINE, M. V. S. Analysis of the feasibility of cardiopulmonary resuscitation during flight in the aircraft of the Paraná Military Police Air Operations Battalion. Recima21 – Multidisciplinary Scientific Journal – ISSN 2675-6218, v. 4, n. 7, p. e473488-e473488, 2023.
MATEUS, P., MARTINS, M., FRUTUOSO, A., FERREIRA, L., & MARTINS, M. Out-ofhospital cardiorespiratory arrest: impact of emergency response time. Management and Development, n. 32, p. 91-107, 2024.
MEDEIROS, A. R., ALMEIDA, E., LOURENÇO, P., SOUSA, V., & LUMINI, M. J. The impact of information systems on the continuity of nursing care. RevSALUS – International Scientific Journal of the Academic Network of Health Sciences of the Portuguesespeaking Countries, v. 6, n. Sup, p. 140-145, 2024.
MELO, C. L., FERREIRA, B. E. S., SILVA, I. V., DE PAULA LUCINDO, N. C., DE PÁDUA, D. A., & CAETANO, G. K. S. Perceptions of nurses working at SAMU regarding the transfer of patient care. Nursing Brazilian Edition, v. 26, n. 303, p. 9845-9853, 2023.
MELO, R. C., CARLOTTO, F. D., FIGUEIREDO, N. M., & RIQUINHO, D. L. Transition and continuity of care from hospital discharge to primary care: a scoping review. Physis: Journal of Collective Health, v. 35, p. e350216, 2025.
MENDES, C. V. A., DA SILVA CORREA, R., DE OLIVEIRA, W. N., & DA SILVA, B. M. Literature review on the main changes that have occurred over time in cardiopulmonary resuscitation. Scientific Journal of Tocantins, v. 1, n. 1, p. 1-10, 2021.
MENDES, S. A., DE ABREU MENDES, S. I. L., MENDES, J. H., DO NASCIMENTO, G. R. M. S., SIQUEIRA, J. P. A., DE ARAÚJO, A. M., & DUTRA, C. R. S. Risk map of ambulances used in pre-hospital care. Electronic Journal of Health Archives, v. 23, n. 11, p. e14686-e14686, 2023.
MENEGAZ, J. D. C., TRINDADE, L. D. L., & SANTOS, J. L. G. D. Entrepreneurship in nursing: contribution to the sustainable development goal of Health and Well-being. UERJ Nursing Journal (Online). p. e61970-e61970, 2021.
MENEGUIN, S., POLLO, B., FERNANDES POLLO, C., & ZORZI SEGALLA, A. V. The role of nurses in rapid response teams in the management of cardiorespiratory arrest: an integrative review. Nursing: Humanized Care, v. 13, n. 1, 2024.
MENOLLI, G. A., SANTANA, C. J., & MARTINS, E. A. P. Acceptability and usability of a handover application for nurses in pre-hospital mobile and in-hospital emergency care. Archives of Health Sciences of UNIPAR, v. 29, n. 1, p. 494-510, 2025.
MINUZZI, D. D. O. M., & DA SILVA PEREIRA, M. Nurses in mobile pre-hospital care: skills, challenges and strategies for visibility. Dom Alberto Health Journal, v. 10, n. 2, p. 21-42, 2023.
MIRANDA, F. G., & GIRON, L. V. Cardiopulmonary and cerebral resuscitation: historical analysis and current practices. National academy of medicine, v. 193, p. 1, 2022.
MITIDIERI, B., BERTOLIN, D., & GABRIEL, S. A. REVISÃO DOS PROTOCOLOS DE ATENDIMENTO À SINDROME CORONARIANA AGUDA E À PARADA CARDIORRESPIRATÓRIA: UMA ANÁLISE COMPARATIVA ENTRE AS DIRETRIZES DA AMERICAN HEART ASSOCIATION E DO MINISTÉRIO DA SAÚDE DO BRASIL. Revista Corpus Hippocraticum, v. 1, n. 1, 2025.
MORAES FILHO, I. M. D., & TAVARES, G. G. Enfermagem atual e futura na promoção da saúde planetária: atuação para o desenvolvimento sustentável. Texto & ContextoEnfermagem, v. 33, p. e20230415, 2024.
MORAIS, B. K. R., da SILVA, E. M., CHAGAS, D. R., de ARAÚJO, S. A., & AMARO, A. Y. G. RESSUSCITAÇÃO CARDIOPULMONAR NA GESTAÇÃO: UMA REVISÃO INTEGRATIVA. Facit Business and Technology Journal, v. 1, n. 60, 2025.
MOUTINHO BOSSO, B. E. A. T. R. I. Z., SOUZA LEITE, D. U. L. C. I. M. E. Y. R. E., SILVA QUEIROZ, A. G., & CÍCERA VIANA, T. T. Knowledge of the nursing team regarding pediatric cardiopulmonary resuscitation in a maternity hospital in a municipality in the interior of the state of Rondônia. Brazilian Journal of Surgery & Clinical Research, v.41, n. 1, 2022.
MROCZINSKI, A. L., GOMES, D. P., ROSALES, R. H., LINO, R. L. B., & GARBUIO, D. C. Effect of cardiopulmonary resuscitation training on knowledge, satisfaction, and selfconfidence in learning among nurses: a quasi-experimental study. Electronic Nursing Journal,v. 25, p. 74071-74071, 2023.
MÜNCHEN, M. A. B., QUINTANA, A. M., & VASCONCELLOS, S. J. L. Coping strategies used by SAMU professionals when faced with the imminent death of patients. Studies and Research in Psychology, v. 22, n. 1, p. 67-85, 2022.
NACER, D. T., SOUSA, R. M. C. D., & MIRANDA, A. L. Outcomes after Out-of-Hospital Cardiorespiratory Arrest of Clinical and Traumatic Origin. Brazilian Archives of Cardiology, v. 120, p. e20220551, 2023.
NASCIMENTO, J. D. S. G., DO NASCIMENTO, K. G., REGINO, D. D. S. G., ALVES, M. G., DE OLIVEIRA, J. L. G., & DALRI, M. C. B. Clinical competence in nursing for highquality cardiopulmonary resuscitation: an integrative literature review. Journal of Nursing of the Central-West Minas Gerais, v. 11, 2021.
NASCIMENTO, L. M. L.; LIMA, A. F. C. Mobile Emergency Medical Service: direct costs with personnel, materials, medications and solutions. Journal of the School of Nursing of USP, v. 59, p. e20250156, 2025.
NATIONAL ASSOCIATION OF EMERGENCY MEDICAL TECHNICIANS; American College of Surgeons. Committee on Trauma. PHTLS : Prehospital Trauma Life Support. 10. ed. Burlington (MA): Jones & Bartlett Learning, p. 784, 2023.
NICOLADELI, A. V. Comparison of the quality of chest compressions between two ventilation frequencies with bag-valve-mask ventilation in a simulated cardiac arrest scenario using an infant mannequin.2023.
NORTE, G. Continuing Education in External Cardiac Compression Using Simulation. Journal of the Portuguese Society of Anesthesiology, v. 31, n. 4, 2022.
NUNES CONCEIÇÃO, J. C., LEMES DA SILVA, C. V., SILVA RAMOS, R., DA SILVA BATISTA, I. A., ALVES NASCIMENTO, D., SILVA RIBEIRO, R. D. J., JESUS, R., SILVA, N. D., LOUISE, E. ., DE JESUS NETA, C. M., BAHIA DOS SANTOS., P. T., ALVES CORREIA., E., DA PALMA DE JESUS, F., & DANIEL ZANONI, R. Implementation of the Mobile Emergency Care Service (SAMU): Challenges of Integration, Regionalization, and Service Qualification. Focus Magazine (Interdisciplinary Studies Journal) , v. 17, n. 4, 2024.
NUNES, P. D. C., CARVALHO, P. V. R. D., ARCURI, R., BELLAS, H., BULHÕES, B., VIANA, J., & JATOBÁ, A. Exploration of the working conditions of river SAMU-192 in crisis scenarios based on resilience in confronting Covid-19 in the Alto Solimões region. Health in Debate, v. 47, n. 139, p. 791-805, 2023.
NUNES, R. M. M., DA SILVA, D. M. F., & JORGE, M. S. B. Building a Fanpage for SAMU-CE: an institutional communication tool. Research, Society and Development, v. 11, n. 1, p. e14811124686-e14811124686, 2022.
OLIVEIRA, C. C. M. D., O’DWYER, G., & NOVAES, H. M. D. Mobile emergency care service performance from the perspective of managers and professionals: a case study in the state of São Paulo, Brazil. Science & Public Health, v. 27, p. 1337-1346, 2022.
OLIVEIRA, T. M. N., MOREIRA, A. C. M. G., & MARTINS, E. A. P. Simulation of cardiopulmonary resuscitation and the knowledge of first responders: a quasi-experimental study. REME-Minas Gerais Nursing Journal. v. 26, 2022.
PARIKH, P., SAMRAJ, R., OGBEIFUN, H., SUMBEL, L., BRIMAGER, K., ALHENDY, M., & BHALALA, U. Simulation-Based Training in High-Quality Cardiopulmonary Resuscitation Among Neonatal Intensive Care Unit Providers. Frontiers in Pediatrics, v. 10, p. 945321, 2022.
PARK, H. J. The Optimal Strategy for Training Cardiopulmonary Resuscitation (CPR) for Healthcare Professionals: A Scoping Review BMC Medical Education, v. 23, p. 412, 2023.
PASSARINI, J. S., SÃO-JOÃO, T. M., DE ALMEIDA, A. O., & DE SOUZA OLIVEIRAKUMAKURA, A. R. Nurses’ knowledge about cardiopulmonary resuscitation. Recien Journal – Scientific Nursing Journal. v. 11, n. 36, p. 472-482, 2021.
PAULA, C. F. B., SANT’ANNA, M. F. B., LUCIO, F. D., POMPEO, D. A., RIBEIRO, R. D. C. H. M., & WERNECK, A. L. Cardiorespiratory arrest in pre-hospital care. Journal of Family, Life Cycles and Health in the Social Context, v. 9, n. 3, p. 608-618, 2021.
PEDROSA, A. R. C.; FERREIRA, Ó. R.; BAIXINHO, C. R. S. L. Transitional rehabilitation care and continuity of patient care as an advanced nursing practice. Brazilian Journal of Nursing, v. 75, p. e20210399, 2022.
PELEK, C. A., FERREIRA SILVA-JUNIOR, M., & MÜLLER, E. V. Level of knowledge about basic life support among health science students. Brazilian Journal of Medical Education, v. 45, p. e078, 2021.
PEREIRA, E. A. T., RIBEIRO, W. A., FASSARELLA, B. P. A., DO CARMO NEVES, K., DE CASTRO FELÍCIO, F., & DA SILVA, A. C. S. Nurse interventions in advanced life support in pre-hospital care. Ibero-American Journal of Humanities, Sciences and Education, v. 10, n. 9, p. 763-784, 2024.
PEREIRA, E. R., & PAES, G. O. Incidents in the context of pre-hospital care by ambulances: contributions to patient safety. Brazilian Journal of Nursing, v. 76, p. e20220657, 2023.
PEREIRA, E. R., DE MELO SOUZA, V., BROCA, P. V., DA SILVA, M. E., DA SILVA, T. C. J., DE ALMEIDA GUILHERME, F. J., HANZELMANN, R. S., & ROCHA, R. G. Nursing care for patients after cardiorespiratory arrest: An integrative review. Research, Society and Development, v. 10, n. 4, p. e9310413861-e9310413861, 2021.
PEREIRA, H. I. C. C. Standardization of post-resuscitation nursing care for individuals who have experienced cardiac arrest, 2024.
PEREIRA, M. G. N., DE ROCO, K. M. W., DE ALMEIDA, C. L., DE LIMA RAVAGNANI, P. A., MOREIRA, A. C. M. G., HADDAD, M. D. C. F. L., & MARTINS, E. A. P. Clinical simulation as a continuing education strategy for nurses in the insertion of the laryngeal mask. Electronic Journal Health Collection, v. 24, n. 9, p. e16705-e16705, 2024.
PEREIRA, S. C., PIRES, M. L. A., MAGRO, P. P. M., DUARTE, T. T. D. P., & MAGRO, M. C. D. S. The effect of active teaching strategies on interprofessional clinical judgment: a quasi-experiment. Brazilian Journal of Nursing, v. 78, p. e20240148, 2025.
PEREIRA, V. B., DE MEDEIROS PEREIRA FILHO, A., ARAÚJO, M. P. P., PARENTE, M. S. P., DE AMORIM, I. A., & DOS PASSOS, S. M. The management of cardiopulmonary arrest (CPA) in the emergency department. Aurum Publishing House, p. 209-226, 2025.
PERERIA, L. Q. F., CARVALHO, J. F. C., KUBELKE, L. R., & GOMES, A. G. C.Management of cardiorespiratory arrest for high school and pre-university students in the municipality of Rio Verde, Goiás State, Brazil. Research, Society and Development, v. 13, n. 9, p. e6713946875-e6713946875, 2024.
PERKINS, G. D., GRÄSNER, J. T., SEMERARO, F., OLASVEENGEN, T., SOAR, J., LOTT, C., & VOORDE, P. V., MADAR, J., ZIDEMAN, D., MENTZELOPOULOS, S., BOSSAERT, L., GREIF, R., MONSIEURS, K. SVAVARSDÓTTIR, H., ZIDEMAN, D. A. European resuscitation council guidelines 2021: executive summary. Resuscitation, v. 161, p. 1-60, 2021.
PIACEZZI, L. H. V., DA COSTA, K. A. L., MAURÍCIO, L. F. S., LOPES, M. C. B. T., OKUNO, M. F. P., MIURA, C. R. M., & CAMPANHARO, C. R. V. COVID-19 pandemic: changes in cardiopulmonary resuscitation. Brazilian Journal of Health Review, v. 4, n. 1, p.2930-2943, 2021.
POMPERMAIER, C., BALENA, B., & GUINZELLI, S. A. C. Emergency medical services: out-of-hospital cardiopulmonary/respiratory resuscitation care. Unoesc Xanxerê Research and Extension Yearbook, v. 5, p. e24210-e24210, 2020.
PORTELA, R. G., DOS SANTOS CARDOSO, R., DE JESUS PEREIRA, G. H., & DE ABREU GONZAGA, P. P. Construction and validation of a scenario for clinical simulation of cardiorespiratory arrest. Electronic Journal Health Collection,v. 25, p. e19585-e19585, 2025.
PORTO, A. C. S., CARNEIRO, A. S., MARINHO, J. G. G., & DE ALMEIDA TAVARES, H. S. Pediatric emergencies: emergency practices and maneuvers in children. Humanities & Innovation, v. 10, n. 24, p. 320-331, 2023.
PORTO, C. F., MENEZES, A. C., TIBÚRCIO, M., VELOSO, J. C., SILVA, J. L. G., PEDROSA, R. B. D. S., & TREVISAN, D. D. Validation of a simulated scenario for advanced life support in a hospital inpatient unit. Text & Context-Nursing,v. 34, p. e20240240, 2025.
PORTO, S. N., RODRIGUES, M. P. G., DE MORAIS RIBEIRO, F. H., DA CRUZ, G. P., & ALVES, M. G. Teaching to save lives: training high school students in cardiopulmonary resuscitation. Science Life Magazine, v. 1, n. 5, p. 1-6, 2024.
PRADO, Y. L., BORGES, L. P., ROCHA, S. L. S., SILVA, J. C. M., DE LIMA, M. G. A.,
DE JESUS SANTOS, T. S., DE MELO, J. M. D., NASCIMENTO, I. F., JOTER, K. P. L., & COSTA, P. H. The importance of basic life support in the initial response to medical emergencies. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 4, p. 15341542, 2024.
PRANDO, C. B., BERNARDES, A. B., LIBÓRIO, A. N. P., & ROSSONI, E. L. Drop in mortality rate, after implementation of SAMU 192 and reform of the SUS in 2006, in the main cities of Espírito Santo, Brazil. Brazilian Journal of Implantology and Health Sciences, v. 6, n. 8, p. 3561-3570, 2024.
PREFECTURE OF ARAGUAÍNA. Clinical care represented more than 50% of SAMU incidents in 2023. Araguaína, 13 mar. 2024.
QUILICI, A. P., TIMERMAN, B., PEIXOTO, E., GONZALEZ, M. M., GIANOTTO- OLIVEIRA, R., MARTINS, C. S. L., & DALLAN, L. A. P. Update of the Brazilian Society of Cardiology’s Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care – 2019. Arq Bras Cardiol, v. 113, n. 3, p. 449-663, 2019.
RAMOS, V. O., & SANNA, M. C. The inclusion of nursing in pre-hospital care: history and current perspectives. Brazilian Nursing Association, v. 58, p. 355-360, 2005.
REIS, G. R.; PEREIRA, R. M. S. The role of the nursing team in cardiopulmonary arrest: a literature review. Aracê Magazine, v. 7, n. 5, p. 24329-24346, 2025.
REIS, K. B. Effectiveness of clinical simulation in training nurses in pediatric cardiopulmonary resuscitation, 2024
REIS, M. H. R., & COSTA, W. D. SAMU in Brazil: the leading role of the nurse on the front lines. 2024.
RIBEIRO, J. L., RODRIGUES, D. E., FERREIRA, D. C., & SOUTO, A. F. The role of the nurse in assisting the patient undergoing therapeutic hypothermia after cardiorespiratory arrest. In: Transforming care: nursing research, p. 60-72, 2023.
RODRIGUES, B. L. G., RODRIGUES, G. B., SANTOS, I. S., & CAMPOS, E. A. D. Level of knowledge of early childhood education teachers regarding urgent and emergency situations in school. Revolua Magazine, v. 1, n. 1, p. 87-95, 2022.
RODRIGUES, B. L. P., DE MONTALVÃO FRANÇA, A. P. F., DE SOUZA, L. R., MORAES, A. C., DE SOUSA, M. L. B., DA SILVA MIRANDA, E. D. S., & DA SILVA TAVARES, E. Knowledge and challenges of the multidisciplinary team in the care of obstetric cardiorespiratory arrest in a health service in the Amazon. Electronic Journal Health Collection, v. 25, p. e19746-e19746, 2025.
RODRIGUES, D. M.; DA SILVA, R. T.; GALHARDO, A. T. Pre-hospital care. Advanced Studies on Health and Nature, v. 18, 2024.
RODRIGUES, R. A., & BARROS, L. M. B. Quantitative analysis of healthcare professionals’ knowledge levels regarding Basic Life Support. Perquirere, v. 21, n. 1, p. 77-90, 2024.
RONCONI, R. W. F. Guidelines, references and protocols in pre-hospital care, rescue and tactical medicine. Brazilian Journal of Emergency Medicine, 2025.
ROSA, P. H. D., Pereira, L. C., Ilha, S., Zamberlan, C., & de Freitas Cáceres Machado, K. Nurses’ perceptions regarding professional practice in the context of mobile pre-hospital care. Nursing in Focus, v. 11, n. 6, 2020.
S SILVA, A. C., OLIVEIRA, A. R., ALVES, E. E. Q., BARBOSA, R. R. S., & DINIZ, H. J. C. Primary care nurses and knowledge about basic life support in cardiorespiratory arrest: a review. Multidisciplinary Journal, v. 38, n. 2, p. 1-16, 2025.
SÁ, L. G. D. S., LIMA, J. K. N., SANTOS, S. P. D. S., TORRES, B. G., DUARTE, V. A., & DE MENEZES, M. C. D. Training hearts: the experience of training in basic life support. Electronic journal extension in debate, v. 11, n. 10, 2022.
SAMPAIO, B. R., DA SILVA, P. H., RODRIGUES, G. L. C., DE PAIVA, H. F., ALMEIDA, G. L., NAGAI, G. N., MIGOTO, J. N., FIGUEIRA, L. A., JÚNIOR, J. P., OLIVEIRA, E. A., CASTELLI, C. C., SILVA., A. G. PAIVA, C. G. P., OLIVEIRA, M. B., MARQUES, P. H. A., HOLANDA, M. A., BITENCOURT., B. R. R., SILVA, R. C., BAESSO, I. B., CUNHA, M. C. V., & LOPES, F. B. P. Updates to Protocols for Advanced Life Support in Drowning Situations. Brazilian Journal of Implantology and Health Sciences, v. 7, n. 1, p. 195-212, 2025.
SAMPAIO, C. U. D. L., & PENHA, A. D. S. I. University Center Dr. Leão; Penha, Aristiany de Sousa. Interpretation of cardiorespiratory arrest rhythms by nurses through electrocardiography: a study with data, 2025.
SANTANA, J. C. B., DUTRA, B. S., MELO, C. L., DOS SANTOS FERNANDES, D., MORAIS, D. A., MARGOTI, F. H., & DARÉ, A. C. D. C. B. Pre-hospital care: Basic and specialized procedures. CRV, 2025.
SANTANA, L. F., DA CUNHA PARIS, M., GABRIEL, K. D. O. F., ROSA, W. F., PETRY, I. L., ALVES, J. N. B., & ROSSA, T. A. The role of nurses in emergency and critical care: an integrative literature review. Brazilian Journal of Development, v. 7, n. 4, p. 35994-36006, 2021.
SANTIAGO JÚNIOR, L. D. S., RIBEIRO DE MELLO, M. E., JOSÉ ANGEL, D., & DA NÓBREGA DANTAS, M. F. Challenges faced by nursing professionals in pre-hospital care: an integrative review. Focus Magazine (Interdisciplinary Studies Journal), v. 18, n. 3, 2025.
SANTOS, I. S. N., DE SOUZA, C. J., SILVINO, Z. R., ESCUDEIRO, C. L., DE ALMEIDA FERREIRA, R., AZEVEDO, T. T., & VILAR, A. M. A. The use of clinical simulation in developing competencies and skills in cardiac arrest for nursing students. Electronic Journal Health Collection, v. 23, n. 7, p. e12972-e12972, 2023.
SANTOS, M. E. F. F., SANTOS, M. A. A., SILVA, P. M., AZINHEIRO, S. S., COSTEIRA, C. R. B., & DUARTE, H. M. S. Theoretical knowledge of nurses regarding advanced life support in the care of critically ill patients. Journal of Nursing Referência, p. 1-9, 2024.
SCABORA, D. M. F. R., SANTIAGO, D. P., SCHIBLER, C. E. M., & INOUE, L. H. Nursing care after cardiorespiratory arrest: an integrative review. Lumen et virtus, v. 15, n. 41, p. 5814-5830, 2024.
SCABORA, D. M. F. R., SANTIAGO, D. P., SCHIBLER, C. E. M., & INOUE, L. Nursing care after cardiopulmonary arrest: an integrative review. Lumen et virtus, v. 15, n. 41, p. 5814-5830, 2024.
SCHLINZ, M. P., TONY, A. C. C., DA COSTA, Y. C. N., ALVIM, A. L. S., RIBEIRO, L., CAVALCANTE, R. B., & DA COSTA CARBOGIM, F. Impact of the evaluator’s presence in clinical simulation of advanced life support: a randomized clinical trial. Nursing Journal UERJ, v. 33, p. e85488-e85488, 2025.
SILVA, A. C., OLIVEIRA, A. R., ALVES, E. E. Q., BARBOSA, R. R. S., & DINIZ, H. J. C. Primary care nurses and knowledge about basic life support in cardiorespiratory arrest: a review. Multidisciplinary Journal, v. 38, n. 2, p. 1-16, 2025.
SILVA, A. J., & DONDA, A. C. The role of the nurse in pre-hospital mobile emergency care. Health of the Valleys Magazine, v. 2, n. 1, 2022.
SILVA, C. S.; OLIVEIRA, G. D. G. C. F. A.; OLIVEIRA, J. S. P. Nurse’s protocol for hospital care in cases of cardiorespiratory arrest. REVOLUA, 2022.
SILVA, G. P.; LIMA, R. P.; GANDRA, E.; SOUZA, E. B. The Role of the Nurse in the SAMU (Emergency Medical Service) Regulation Center: A Literature Review. National Conference on Trauma and Emergency Medicine,v. 3., 2024.
SILVA, J. P., DE ANDRADE, I. C. A., DOS SANTOS, E. E. C., SILVA, C. D. J. M. S., PANTOJA, J. P., SANTIAGO, G. M., & MESQUITA, C. R. Early recognition of stroke and cardiac arrest: first aid actions that save lives. Electronic Journal of Health Archives, v. 25, p. e18937-e18937, 2025.
SILVA, L. D. C., FERREIRA, N. S., DE ARAÚJO COSTA, T. V., NUNES, F. D. O., DIAS, R. S., & AZEVEDO, P. R. Cardiovascular emergencies handled by the mobile emergency medical service. Vale Magazine,v. 23, n. 2, 2025.
SILVA, M. P. B., LEITE, A. C., DE CARVALHO, S. B., DE CARVALHO, M. B., LIMA, M. S., PENHA, C. M. S. D., & DE REZENDE, A. O. The multidisciplinary team facing a patient who is a victim of cardiorespiratory arrest. Research, Society and Development, v. 9, n. 11, p. e3119119761-e3119119761, 2020.
SILVA, M. P. B., LEITE, A. C., DE CARVALHO, S. B., DE CARVALHO, M. B., LIMA, M. S., PENHA, C. M. S. D., SILVA, J. M. I., BARRADAS, K. L., SOUSA, J. F., COUTINHO, L. A., LIMA, J. H. C., SCHUSTER, A. L., BASSANI, B. F. B., COSTA JÚNIOR, V. L., ALMEIDA, R. C., LOPES, J. R., & DE REZENDE, A. O. The multidisciplinary team facing a patient who is a victim of cardiorespiratory arrest. Research, Society and Development, v. 9, n. 11, p. e3119119761-e3119119761, 2020.
SILVA, N. M., GIL, A. B., BRITO, J. N. M., DO NASCIMENTO LEITE, S. J., & BITENCOURT, A. L. S. Development of educational technology for the management of cardiorespiratory arrest in pediatrics. JRG Journal of Academic Studies, v. 8, n. 18, p. e181822-e181822, 2025.
SILVA, S. M., & LIMA, R. N. Nursing leadership in in-hospital adult cardiopulmonary arrest (CPA). Ibero-American Journal of Humanities, Sciences and Education, v. 8, n. 11, p. 1177-1185, 2022.
SOAR, J., BÖTTIGER, BW, CARLI, P., COUPER, K., DEAKIN, CD, DJÄRV, T., & NOLAN, JP. European Resuscitation Council Guidelines 2021: Adult advanced life support. Resuscitation, v. 161, p. 115-151, 2021.
SOUSA, B. V. N., TELES, J. F., & OLIVEIRA, E. F. Profile, difficulties and peculiarities in the work of professionals in mobile pre-hospital care services: an integrative review. Nursing Today of Costa Rica, n. 38, p. 245-260, 2020.
SOUSA, D. C.; SILVA, J. D. Geolocation applied to SAMU 192 emergency services based on real-time tracking of ambulances. Brazilian Journal of Health Informatics. 2018.
SOUSA, Y. V. L.; DE CARVALHO BORGES, L. S.; VELOSO, L. C. Nursing assistance in cardiopulmonary arrest in the Mobile Emergency Medical Service (SAMU).Research, Society and Development, v. 10, n. 6, p. e6510615651-e6510615651, 2021.
SOUZA, M. S., DA SILVA, D. M., MAIA, M. A., VENTURA, P. F. E. V., & ALVES, M. Organization of the daily work of Mobile Emergency Care Service professionals. Pedagogical Notebook, v. 21, n. 13, p. e12681-e12681, 2024.
SOUZA, R. M. D., MORABITO, R., CHIYOSHI, F. Y., & IANNONI, A. P. Analysis of SAMU configuration using multiple ambulance location alternatives. Management & Production, v. 20, p. 287-302, 2013.
STEFANI, G. A. Experiences of nurses in advanced practices in mobile emergency medical services. 2021.
TACAHASHI, D. S., PIRES, A. A., & SILVANIO, D. A. R. Emergency cart: nursing team’s knowledge regarding its composition, organization, and handling. Journal of the Faculty of Medical Sciences of Sorocaba, v. 27, n. Fluxo contínuo, p. e64945-e64945, 2025. TACAHASHI, D. S.; PIRES, A. A.; SILVANIO, D. A. R. Emergency cart: nursing team’s knowledge regarding its composition, organization, and handling. Journal of the Faculty of Medical Sciences of Sorocaba, vol. 27, continuous flow, p. e64945-e64945, 2025.
TAMINATO, M., FERNANDES, H., & BARBOSA, D. A. Nursing and the Sustainable Development Goals (SDGs): An essential commitment. Brazilian Journal of Nursing, v. 76, p. e760601, 2023.
TAVEIRA, R. P. C.; SOUZA, M. F.; SILVA, J. C,; ALMEIDA, A. L.; PEREIRA, C. H. Nurses’ Role in Pre-Hospital Emergency Care. Global Academic Nursing Journal, [S. l.], v. 2, n. 3, p. e156, 2021.
THANNHAUSER, J. An update on technical innovations in the prehospital chain of survival. Prehospital Emergency Care, 25(5), 673-680, 2021.
TOFANI, L. F. N., FURTADO, L. A. C., ANDREAZZA, R., NASSER, M. A., BIZETTO, O. F., & CHIORO, A. The Emergency Care Network on the Scene: Contingencies and Care Delivery. Health in Debate, v. 46, p. 761-776, 2022.
TORRENTE, G., GARCIA, L. C., TONAKI, L., DE SOUZA, G. L. I., BARBOSA, L. M. D. C. P., DE SOUZA, T. Q., & DA SILVA, G. Mobile pre-hospital care and technology: a validation study. Journal of Health Informatics, v. 16, n. Especial, 2024.
TSAO, CONNIE W.; ADAY, AARON W.; ALMARZO OQ, ZAID I.; ANDERSON, CHERYL A. M.; ARORA, PANKAJ; AVERY, CHRISTY L.; BAKER-SMITH, CARISSA M.; BEATON, ANDREA Z.; BOEHME, AMELIA K.; BUXTON, ALFRED E.; COMMODORE-MENSAH, YVONNE; ELKIND, MITCHELL S. V.; EVENSON, KELLYR.; EZE-NLIAM, CHETE; FUGAR, SETRI; GENEROSO, GIULIANO; HEARD, DEBRA G.; HIREMATH, SWAPNIL; HO, JENNIFER E.; KALANI, RIZWAN; KAZI, DHRUV S.; KO, DARAE; LEVINE, DEBORAH A.; LIU, JUNXIU; MA, JUN; MAGNANI, JARED W.; MICHOS, ERIN D.; MUSSOLINO, MICHAEL E.; NAVANEETHAN, SANKAR D.; PARIKH, NISHA I.; POUDEL, REMY; REZK-HANNA, MARY; ROTH, GREGORY A.; SHAH, NILAY S.; ST-ONGE, MARIE-PIERRE; THACKER, EVAN L.; VIRANI, SALIM S.; VOEKS, JENIFER H.; WANG, NAE-YUH; WONG, NATHAN D.; WONG, SALLY S.;YAFFE, KRISTINE; MARTIN, SETH S.; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2023 update: a report from the American Heart Association. Circulation, [S. l.], v. 147, n. 8, p. E93-E621, 21 fev. 2023.
TURRA, L., LAZZARI, D. D., MARTINI, J. G., NASCIMENTO, E. R. P. D., RAMOS, F. C., MALFUSSI, L. B. H. D., BECKER, A., & MENDES, N. U. Knowledge of the nursing team about cardiopulmonary arrest and resuscitation: mixed methods studies. Gaucho Journal of Nursing, v. 45, p. e20230280, 2024.
VASCONCELLOS, R. N., SANTOS, D. C., DA SILVA MENDES, J. A., DOS SANTOS CARDOSO, L. P., ALVES, L. B., & PEREIRA, J. A. The role of the nursing team in the face of cardiorespiratory arrest in the hospital setting: an integrative review. Remecs Journal – Multidisciplinary Journal of Scientific Studies in Health., p. 32-32, 2021.
VERVLOET, M. M., BARBOSA, P. M. D. S., FRANCISCO, D. V., & CABRAL, P. E. The role of nursing in unassisted cardiopulmonary arrest (CPA). Multidisciplinary Scientific Journal, Knowledge Center,v. 7, n. 06, p. 106-119, 2022.
VESTERGAARD, L. D., LAURIDSEN, K. G., KRARUP, N. H. V., KRISTENSEN, J. U., ANDERSEN, L. K., & LØFGREN, B. Quality of Cardiopulmonary Resuscitation and 5-Year Survival Following In-Hospital Cardiac Arrest. Resuscitation, v. 167, p. 112-120, 2021.
VICENTE, D. A. R., FARIA, A. S., DE CARVALHO, E. B., MATANA, G. A., DE SOUZA AMARAL FILHO, J. E., ROCHA, L. A., & CABRAL, R. F. R. P. Pacientes em parada cardiorrespiratória em ambientes intra e extrahospitalar. Brazilian Journal of Health Review, v. 7, n. 1, p. 972-994, 2024.
VIEIRA, J. W., & DELL’AGNOLO, C. M. Prehospital care in the mobile emergency care service in Northwest Paraná: response time and determining factors according to drivers. Electronic Journal of Nursing Archives, v. 18, p. e10116-e10116, 2022.
VIEIRA, O. L. G. F., DE BRITO MEIRA, F., & DOS SANTOS MARINHO, M. The importance, limitations and difficulties of SAMU 192: an integrative literature review. UNILUS Teaching and Research, v. 18, n. 51, p. 279-286, 2021.
VINAGRE, R. C. Recognition by the Medical Regulator of the Expressions Used by Laypeople When Requesting Help in Cases of Suspected Cardiorespiratory Arrest. Brazilian Archives of Cardiology, v. 121, n. 11, p. e20240669, 2024.
WALENDOWSKY, A. S. S. R. Minimum Viable Product of a visual communication system for patient safety in cardiopulmonary resuscitation. 2025.
WEIL, M. H.; TANG, W. Endotracheal drug administration during cardiopulmonary resuscitation. Crit Care Med., v. 28, n. 6, p. 2144-2146, 2000.
WIK, L., KRAMER-JOHANSEN, J., MYKLEBUST, H., SØREBØ, H., SVENSSON, L., FELLOWS, B., & STEEN, PA. Quality of Cardiopulmonary Resuscitation During Out-ofHospital Cardiac Arrest. Journal of the American Heart Association, v. 10, n. 3, e018123, 2021.
WINTER, B. L., SULCZEWSKI, I., DAL’SOTO, L. F., RIBEIRO, M. S., & BENETTI, E. R. R. Nursing care in cardiorespiratory arrest in an in-hospital emergency setting: student experiences. In: Production of knowledge in nursing and health: sharing experiences of students and professors. Scientific Digital Publisher, p. 91-102, 2023.
XAVIER, L. F., & DE SOUSA, D. A. Nursing care for patients in cardiorespiratory arrest: an opinion piece. Nursing Brazil, v. 23, n. 6, p. 2119-2126, 2024.
ZOSCHKE, C. F. T. S., KUZNIER, T. P., BETIOLLI, S. E., DE ALMEIDA CRUZ, E. D., FELISBINO, K., DE ALMEIDA HAMMERSCHMIDT, K. S., & GARCIA, R. B. F. Manual defibrillation by nurses in cardiopulmonary resuscitation: an integrative review. Nursing Brazilian Edition, v. 29, n. 319, p. 10392-10398, 2025.
¹ Maurício de Nassau University Center, Av. Augusto Franco Avenue, 2340, 49075-470, Aracaju, Brazil.
² Tiradentes University. Av. Murilo Dantas, 300, 49010-390 Aracaju, Brazil
³ Institute of Technology and Research and Tiradentes University. Av. Murilo Dantas, 300, 49010-390 Aracaju, Brazil e.mail: enf.jennifernascimento@outlook.com
